Lesson 3: How To Avoid SARS-CoV-2 Infection
Lesson 3 Protocol 1
To routinely do the six things that can keep you from getting infected, as describe below and in the Action(s) tab.
Remember that prevention is the best cure for COVID-19.
The most reliable way to not get infected with SARS-CoV-2 and then potentially have to deal with a difficult COVID-19 illness is to:
- Wash your hands regularly with soap.
- Not touch your face, especially your eyes, nose or mouth.
- Wear a highly rated, clean face mask in public.
- Socially distance 6 feet (2 meters) apart.
- Ventilate your home.
- Use a nasal spray inhaler when in public.
How To Avoid SARS-CoV-2 Infection
During this pandemic, the best thing you can do is to not test your immune system against this virus.
Don’t get infected!
This message needs to be internalized by everyone, even the young and healthy.
Don’t be that 30-year-old Texan, who just before he died in mid-July after attending a so-called a COVID-19 hoax party said, “I think I made a mistake”.
No matter how young and healthy you are, take the precautions needed to avoid getting infected.
We’re going to cover the six ways you can avoid getting infected with SARS-CoV-2, and thereby potentially suffer through any Covid-driven disease.
I’ll tell you about these in a moment, but first I want to cover how transmission of this virus happens so that you can protect yourself.
SARS-CoV-2 Transmission
As you know, SARS-CoV-2 is a highly contagious virus that’s transmitted from person to person by:
Droplets of different sizes transmitted from person to person within 6 feet (2 meters) of each other should one have symptoms.
Airborne transmission of droplet particles that can remain in the air for long periods of time and be transmitted to others over distances greater than 6 feet (2 meters). They float and follow the air streams in a room.
Contact with surfaces in the immediate environment, or by objects used by an infected person.
Details about airborne transmission are still being hammered out. The data about how long droplet particles can remain in the air, and the distance of transmission were determined in a laboratory setting, and that may not mirror real life situations. [1]
It’s pretty clear, however, that droplets and droplet particles can enter your eyes, nose or mouth. People have gotten the virus via droplet particle transmission. People in a restaurant in China who sat downstream from an air conditioner caught COVID-19.
Let’s use cigarette smoke to analogize droplets and droplet particles. You can think of droplets and droplet particles like cigarette smoke. If you’re next to a smoker, you get plumes of smoke in your face, the smell is strong, and you inhale a lot of it. This is like being within six feet of someone without a face mask, in which case you might get droplets in your eyes, nose or mouth.
The droplet particles experience is more like entering a room where a smoker has recently been smoking. You can smell it, and you can inhale it, but less of it than if you were near a person smoking.
And at a choir practice in Washington state, many choir members got sick with coronavirus after breathing in tiny airborne particles generated by individuals who were infected but symptom-free at the time.
Personally, I’m risk averse enough to want to have a mask on when I enter a building where people have been even if no one is presently near me.
Now, you might think, “Well, this building has good ventilation, so I won’t wear my mask”. You could be right, but only if the ventilation system has adequate filtration and brings in fresh air from outside.
Most likely, you’re not going to know that.
Now let’s turn to kids.
When this coronavirus pandemic began, epidemiologists thought that basically children we’re pretty much immune. They could get the virus, but their immune system would keep them asymptomatic.
That remains pretty much true, unless children -- like adults -- have some comorbidity that makes them vulnerable.
Unfortunately, in the U.S. nearly 19% of children between 2 and 18 years old are obese, and that’s a big confounding factor, because it increases such a child’s risk for COVID-19.
But there’s another problem -- kids are virus spreaders.
Children can carry at least as much of the coronavirus in their noses and throats as adults. They are adept at spreading other kinds of viruses, including the flu, and the same goes for the coronavirus. [2]
As long as we’re on the topic of kids getting infected, let’s look at a snapshot of who else is vulnerable to getting SARS-CoV-2. A useful case study is the breakdown of who was infected in a resurgence of the virus in San Francisco in late July 2020. Nearly half of all cases reported in San Francisco residents were between the ages of 18 and 40, with:
So you can see that older people aren’t the only vulnerable demographic. In fact, the average age of those hospitalized at the San Francisco’'s Zuckerberg General is just 41 years old. [3] Lesson 10 delves deeper into the specific health issues that make people vulnerable to this virus, but before we get there, there’s much you need to know about how to avoid a SARS-CoV-2 infection. |
The six ways to avoid SARS-CoV-2 infection are to:
- Wash your hands regularly;
- Don’t touch your face;
- Wear a face mask when indoors with other people, other than in your home;
- Keep a physical distance of six feet from others when indoors (about 2 meters);
- Ventilate your indoor space; and
- Use a saline-based nasal inhaler regularly when outside your home.
There’s good science behind each of those six methods to avoid infection. The ones you prioritize should depend on your personal risk profile.
Let’s begin with the easiest thing to do -- wash your hands.
Wash Your Hands
The reason you want to wash your hands regularly is because we touch our face all the time. If the virus is on your hands, touching your face is a good way to get infected.
Respiratory viruses — like the novel coronavirus, the flu, and the common cold — can be spread via our hands. If someone is sick, a hand can touch some mucus and viral particles will stick to it.
Hands act like sticky traps for viruses. We can pick up droplets that contain the virus, and they’ll stay on our hands, and enter our bodies if we touch our face.
That’s why washing our hands frequently is so important in the war against COVID-19. The Centers for Disease Control and Prevention (CDC) recommends washing your hands with soap and water as the best way to clean them. But if soap and water are not available, using a hand sanitizer with at least 60% alcohol will help.
When you wash your hands with soap, the fat emulsifiers in the soap disintegrate the virus. That’s because much of it is fat. The depiction below shows incoming fat emuslifiers (aka "soap") that destroys the virus.
Think of the virus as bits of genetic information — encoded by RNA — surrounded by a coat of fat and protein. Basically, they’re “nano-sized grease balls.” And grease balls, no matter the size, are what soap loves to annihilate.
As you wash your hands, the harmless shards of virus get flushed down the drain. And even if the soap doesn’t destroy every virus, you’ll still rid them from your hands with soap and water, as well as any grease or dirt they may be clinging to.
Soap will also wash away bacteria and other viruses that may be a bit tougher than coronavirus, and harder to disintegrate.
Spend 20 seconds washing your hands, about the time it takes to sing happy birthday twice.
When I first began to frequently wash my hands during this pandemic, I sang happy birthday to my sister, whose birthday was coming up at the time. I did this twice in successions, which takes about 20 seconds, the amount of time suggested you spend washing your hands.
After her birthday came and went, I chose to sing to another friend whose birthday was approaching. Given that I’m a compassionate person, I don’t sing out loud.
Don’t Touch Your Face
The virus can only infect you if it can get inside you. Having the virus on your fingers is only a problem if you move that virus from your fingers to your eyes, nose, or mouth…. or someone else’s.
It’s not that touching your face anywhere is the problem-- touching your forehead, cheek, or chin is not much worse than touching your forearm.
The virus can’t pass through your skin. The virus can only replicate in live cells, and the outer layer of your skin is covered by protective strata of dead skin cells.
To get into your lungs and elsewhere, the virus has to find its way to your mucous membranes, the moist lining of your nostrils, mouth or eyes. You can avoid this possibility simply by getting into the habit of not touching your face.
Not touching your face is a huge challenge, because it’s something we all do a lot. On average, we touch our eyes, nose or mouth 10 to 16 times an hour.
Unless you want to wear a catcher’s mask all the time, the only reasonable way to keep yourself from touching your eyes, nose or mouth is to become aware of these unconscious acts and try to stop them.
If a catcher’s mask doesn’t suit you, you can wear a mask and glasses all the time.
No one wants to do that, so instead, become aware of how often you touch your face and stop it, and wash your hands a lot, so that when you inevitably do touch your face, it will be with virus-free fingers.
Wear A Face Mask
Wearing a face mask while indoors with people milling around is the second thing to do to avoid infection.
The science clearly shows that face masks can prevent coronavirus transmission and save lives.
An analysis of 200 countries found that places where masks weren't recommended saw a 55% weekly increase in coronavirus deaths per capita after their first case was reported, compared with 7% in countries with cultures or guidelines supporting mask-wearing. [4]
A model from the University of Washington predicts and compares the prevention of coronavirus deaths in the U.S. if 95% of the population were to wear face masks in public versus current trends of mask wearing.
The model is dynamic; it changes as new data is inputted, but there’s a notably higher number of deaths that happen when masks are not worn in public.
The CDC recommends that you wear a face mask when outside, especially if you’re in an enclosed area with others, or where people might have been recently. This is not only to protect yourself from others who might be infected with COVID-19, but to help you not spread the virus if you’re infected, but don’t realize it, which means you’re asymptomatic.
Assuming your mask is made of protective materials, the obvious protection it offers is to block or substantially reduce the viral load that could spew out of an infected person’s mouth while coughing, sneezing or talking close to you.
But there are three less obvious reasons why wearing a mask protects you:
- Low humidity
- Public restrooms
- Airborne dust
Low humidity is a key factor in the spread of the Coronavirus. Scientists estimate that for a 1% decrease in relative humidity, COVID-19 cases increase by 7 to 8%. [5]
When the humidity is lower, the air is drier and it makes the aerosols smaller. Since aerosols are smaller than droplets, when you sneeze and cough, those smaller infectious aerosols can stay suspended in the air longer than droplets. This increases the exposure for other people. When the air is humid and the aerosols are larger and heavier, they fall and hit surfaces quicker.
I’ll speak to how to increase the humidity in your nasal passages later.
What about public restrooms? Yes, their havens for the virus.
Scientists simulated and tracked virus-laden particle movements when toilets and urinals were flushed. They discovered that flushing involves an interaction between gas and liquid, resulting in a large spread of aerosol particles.
The trajectory of the particles ejected from flushing showed that more than 57% of the particles traveled away from the urinal. [6]
The third reason a mask protects you is to keep you from breathing in viruses that can spread through the air on dust, fibers and other microscopic particles.
This was studied by counting airborne particles given off dust aerosolized by guinea pig movement rather than respiratory droplets from their breath. The researchers found spikes of up to 1,000 particles per second came off the animals as they moved around their cage. [7]
Guinea pigs immune to influenza had the virus applied to their fur. They transmitted the virus through the air to other, not-immune guinea pigs, showing that the virus did not have to come directly from the respiratory tract to be infectious.
The researchers also tested whether microscopic fibers from an inanimate object could carry infectious viruses. They treated paper facial tissues with influenza virus, let them dry out, and then crumpled them in front of an automated particle sizer.
Crumpling the facial tissues released up to 900 virus particles per second in a size that could be inhaled. The researchers were also able to infect cells from these particles released from the virus-contaminated paper tissues.
Clearly, it’s in your self interest to wear a face mask, and it’s the responsible thing to do for others, because you may be infected and not know it.
We know from recent studies that a significant portion of individuals with coronavirus lack symptoms, and that even those who eventually develop symptoms can transmit the virus to others before showing symptoms. [8]
Face masks do not replace the need for washing hands or social distancing, nor do they alone prevent the spread of COVID-19. What masks do really well is to help reduce the chance of infecting others if you’re sick, and don’t know it.
The pertinent question is which mask does the job best? They don’t all offer the same level of protection for you, or others near you.
The ideal face mask blocks large respiratory droplets from coughs or sneezes – the primary method by which people pass the coronavirus to others – along with smaller airborne particles, called aerosols, produced when people talk or exhale.
Check out a quick example of this offered by "Bill Nye the Science Guy":
Bill Nye showed you how a simple double layer of cloth can keep you from spreading viral particles, but let’s delve deeper into the most protective face masks, both for you, and those around you.
The N99 and N95 offer the best protection for filtering viral particles. Both of these masks seal tightly around the nose and mouth so that very few viral particles can seep in or out. They also contain tangled fibres to filter airborne pathogens.
A study published in the Journal of Hospital Infection evaluated more than ten masks based on their ability to filter airborne coronavirus particles. [9]
The researchers found that N99 masks reduced a person's risk of infection by 94 to 99% after 20 minutes of exposure in a highly contaminated environment, and the N95 masks offered almost as much protection.
Second place went to disposable surgical masks. Surgical masks are made of nonwoven fabric, so they're usually the safest option for healthcare workers who don't have access to a N99 or N95 mask. Surgical masks are about three times as effective at blocking virus-containing aerosols than homemade face masks.
Then, of course, there’s a bewildering number of face masks offered by various manufacturers. Or you can make your own.
The best-performing home made design is constructed of two layers of high-quality, heavyweight “quilter’s cotton” with a thread count of 180 or more, and those with especially tight weave and thicker thread, such as Batik quilting fabrics.
A double-layer mask with a simple cotton outer layer and an inner layer of flannel also performed well.
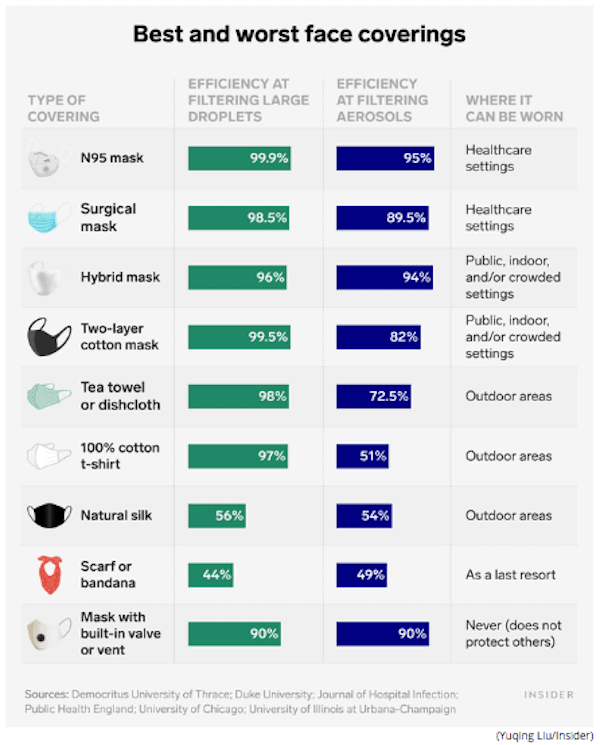
Whether you buy one or make your own, make sure you use the most protective fabric. Here’s a ranking of the best and worst face coverings based on the latest research:
If you choose to use a surgical mask, make sure it fits. Here’s a tip for doing that, demonstrated by Dr. Olivia Cui.
If you intend to make your own mask, make sure you use the most protective materials. Keep that in mind when you watch this video by Dr. Jerome Adams, the Surgeon General of the United States.
He demonstrates how to make the simplest mask I’ve seen that can prevent infection, but you can choose to use more protective materials than shown in his examples.
Whatever mask you choose to use, make sure it meets the CDC’s criteria. It must:
- Fit snugly (but comfortably) against your face.
- Be secured with ties or ear loops.
- Include multiple layers of fabric.
- Allow for breathing without restriction.
- Be washable without damage or shape change.
Keep Your Distance

A sneeze can carry the coronavirus pathogen in droplets and in aerosols — and they could land on a surface, making it a fomite.
We’re told to keep some distance apart from others so that virus particles from one or more people don’t reach our eyes, nose or mouth.
Six feet (or about 2 meters) apart is the recommendation for physical distance between you, and those you aren’t living with, but there’s more to consider.
The World Health Organization has formally recognized that SARS-CoV-2, is airborne, and that it can be carried by tiny aerosols.
When we cough and sneeze, talk or just breathe, we release into the air small particles of fluid referred to as “droplets”, which we’ve covered, but what’s also emitted are smaller particles of fluid referred to as “aerosols”.
Aerosols can be as infectious when transmitted through direct contact, or by droplets released at close range.
The concern here is that you walk into a small room that an infected person was just in. Obviously, that person was breathing while in the room. Now he or she is gone, but the virus particles linger in the air via those droplets and aerosols. You can breathe them in and get infected.
A New York Times article that provides some details about this. The bottom line is that virus particles in aerosols and droplets can linger in the air, and drop onto and infect furniture, table tops and the like.
Protect yourself by frequently washing your hands, wearing a mask, social distancing, and -- as we’ll cover next -- ventilating and using a nasal spray inhaler.
Ventilate
A straightforward formula for calculating the risk of getting the SARS-CoV-2 virus is:
Risk of infection = volume of exposure + time exposed
The greater the volume of viral particles you’re exposed to, and the longer you are exposed to them, the higher your risk of infection.
This formula helps to understand why the three major preventative measures -- social distancing, masks, and hygiene -- are effective.
Let’s add another protective element: ventilation! The idea here is simple: reduce the chances that the air you breathe contains the virus.
We know that the risk of getting the coronavirus is much lower outdoors than indoors, and this is largely due to ventilation.
When outdoors, exhaled viral particles disperse quickly into the air, thus reducing the volume of exposure.
In indoor environments, especially when poorly ventilated, the viral particles don’t disperse, so the volume of exposure is much higher. The more time you spend indoors, the more important is proper ventilation.
This might explain why adults who got coronavirus are twice as likely to have dined out, says the CDC. [10]
When viral particles escape into indoor air, we have two options for reducing exposure:
- Bring fresh air in from outside.
- Remove the virus from indoor air.
Let’s talk about bringing fresh air in from outside first.
You can’t do anything about the adequacy of the Heating, Ventilation, and Air-Conditioning systems in commercial buildings you may enter, but you can get more ventilation into your home.
The best way to bring outside air inside into your home is to open the windows, if the climate allows. The more fresh, outside air the better. Most building scientists recommend at least six changes of air per hour in a 10x10 foot room (or 3x3 meters) with four people in it. [11] During a pandemic, however, some recent studies suggest that nine changes per hour is better. [12]
One way to know if you’re getting enough air exchange is to measure CO2 (carbon dioxide) levels. A well-ventilated room will have CO2 levels of 800 ppm or below.
A study at Taipei University in Taiwan looked at how indoor ventilation affected a tuberculosis outbreak. Many of the classrooms had poor ventilation, with CO2 levels of 3,000 ppm or higher. [13]
When ventilation was improved to where CO2 levels dropped below 600 ppm, the outbreak was completely stopped.
Unfortunately, many schools and workplaces don’t have adequate ventilation. If you’re considering whether to return to work, or whether to send your kids back to school, you might want to measure the CO2 levels in the indoor spaces.
You can buy a CO2 monitor online. A room needs more ventilation if CO2 levels are higher than 800 parts per million. This can be done by increasing the amount of outside air the Heating, Ventilation, and Air-Conditioning system brings in, if there is one, or by opening windows.
The other option is to remove the virus from the indoor air. The best way to do this is with a high-quality HEPA air filter.
I’ve placed links in the Resources tab for a CO2 monitor, a HEPA air filter that filters particles as small as 0.003 microns, which are smaller than viruses; and a filtration system for the whole house.
Now to the last way to prevent infection in our list, a nasal spray inhaler.
Use A Nasal Spray Inhaler
Using a spray inhaler departs from the five other basic strategies we covered, because using an inhaler will not prevent contact with the virus. What it can do, however, is to prevent the virus from infecting you and getting you sick.
A review of three studies about COVID-19 underscored the importance of clearing your nasal cavity of the virus before it can do much damage. By using an nasal spray inhaler, specifically a brand called Xclear, the researchers found that the virus was reduced to an undetectable amount in 15 minutes. [14]
This study was replicated at Geneva University. And another study done by researchers at the University of North Carolina, Chapel Hill supports the claim that cleansing the virus from the nasal cavity before it firmly establishes itself before moving on to the respiratory system is an effective way to block infection or lessen the severity of symptoms.
It appears that the major reason a nasal spray can be effective in clearing a virus from the nasal cavity is due to humidity.
A study published in 2019 looked at the role of humidity in our respiratory tract can confer immunity to influenza virus. The researchers saw that a 40 to 60% relative humidity helped remove the virus from the respiratory tract. [15]
So, it appears that keeping the nasal cavity humid is a good thing to do.
When I’m going to be out among people indoors I use Xlear, the product tested in the Utah State University nasal spray study. When in close proximity to others for more than a few minutes, I give myself a nasal blast every hour. Again, the objective is to make the nasal passages more humid and thereby help clear the virus.
Your Takeaway
Remember that prevention is the best cure for COVID-19.
Do your best to:
- Wash your hands regularly with soap.
- Not touch your face, especially your eyes, nose or mouth.
- Wear a highly rated, clean face mask in public.
- Socially distance 6 feet (2 meters) apart.
- Use a nasal spray inhaler when in public.
Next up in Lesson 4 is the second step to take to build your foundational immunity, which is to reduce your baseline inflammation.

Leave a comment
Comment as a guest: