How To Survive The Coronavirus Outbreak (COVID-19)

To survive the coronavirus outbreak (COVID-19) that is sweeping across the globe, you must be vigilant and prepare. In this post, I list the risk factors and tell you how to prepare.
Check out my Covid Immunity CourseFace Mask Update on April 20, 2020 See NYT's Live Updates and John Hopkins' Daily Reports
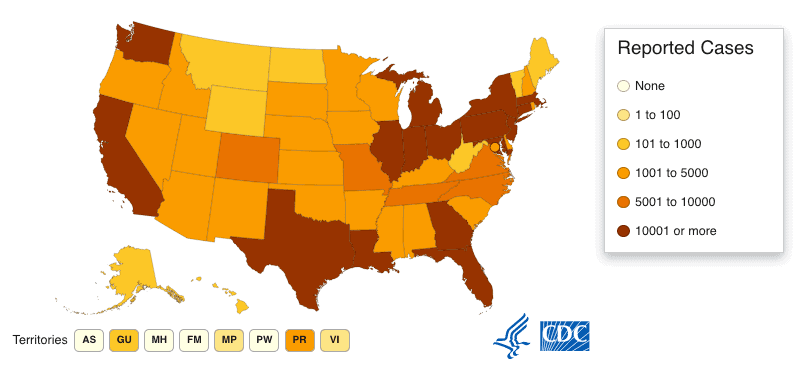
CDC infection map (how’s your state doing?) ✔
Hydroxychloroquin/Remdesivir: yes or no? (new info) ✔
What’s going on with testing? (new info) ✔
What are the symptoms (video showing how infection occurs)
Masks are now mandatory in some cases (make your own with this video)
Learn how to make your immune system more robust
CDC Reported COVID-19 Cases in the USA, 4/20/2020
- Total cases: 746,625 (last week: 492,416)
- Total deaths: 39,083 (last week: 18,559)
Top 5 States with Most Infections (cases reported):
(These numbers will be outdated by the time you read them, so fast are infections spreading.)
New York: 238,138 (was 157,073 last week)
New Jersey: 85,301 (was 51,027 last week)
Massachusetts: 38,077 (was 18,941 last week)
Pennsylvania: 32,284 (first time in top 5)
Illinois: 30357 (first time in top 5)
Note: California, the USA’s largest state, dropped out of the top five, with 28,963
Go here for updates and to see your state.
Get your daily John Hopkins University of Medicine COVID-19 briefing here.
Go here for daily John Hopkins Situation Reports
The Politics and Policy of COVID-19
John Hopkins-affiliated experts discuss the politics of the information environment around COVID-19, including what social science tells us about how public health communications work, what governments, media and platforms can do to counter misinformation, and how COVID-19 compares to other public health issues, such as gun violence or vaccines.
Interview with John Hopkins Infectious Disease Expert Amesh Adalja, MD
This very informative interview puts things in perspective; meaning, there’s a lot of nuance regarding who is at risk and what level of concern is appropriate. The expert is Amesh Adalja, MD, an infectious disease specialist at the Johns Hopkins University Center for Health Security. His work is focused on emerging infectious disease, pandemic preparedness, and biosecurity.
How frightened should you be? Well, as the above video explains, the answer to that depends on where you live, how much contact you have with other people, your age and how healthy you are, among other things. That said, surely it’s time to learn what’s going on with this coronavirus outbreak, assesses your risk of getting infected by the coronavirus, and prepare to minimize that risk.
As you’ll soon see, I’ve attempted to provide you with enough current information to make a reasoned decision about what to do. Note that you’ll encounter some dramatically different perspectives about the impact that this particular coronavirus outbreak — called COVID-19 — will have in the U.S. My view is to listen to those that have “been there, done that”, such as Bill Gates, and leaders of the Centers for Diseases Control (CDC) or the World Health Organization.
Hydroxychloroquine: An Untested COVID-19 Drug
The CDC’s online advice for Hydroxychloroquine, Remdesivir and other drugs was updated April 13, 2020, and leads with:
There are no drugs or other therapeutics approved by the US Food and Drug Administration to prevent or treat COVID-19.
The U.S. Centers for Disease Control and Prevention (CDC) had abruptly switched its guidance for use of a drug touted by President Donald Trump as a possible treatment for COVID-19, dropping its reference to anecdotal dosages, and underscoring that there are no approved drugs for dealing with the disease.
Bill Gate’s COVID-19 Perspective and Video Interview
Bill Gates said that this coronavirus may be the “once-in-a-century pathogen we’ve been worried about,” and pointed out that COVID-19′s current predicted fatality rate is higher than that of the 1957 influenza pandemic, which killed an estimated 66,000 people in the U.S.
Bill was interviewed for TED Talks on March 24, 2020 and made these important points:
- Even though COVID-19 has a far lower mortality rate than SARS or smallpox, it has devastated the world due to its far higher infection rate.
- What’s disarming about respiratory infections like COVID-19 is that people infected don’t initially know their sick, and therefore still go about their lives infecting others.
- Tests exist that can be self-administered, instead of by a health worker, therefore dramatically improving widespread testing. But right now such tests are a rarity. Bill expects that this might change within a few weeks.
- Testing and isolation go hand-in-hand, because if you know you’re infected you can isolate yourself and not infect others.
- South Korea did not have to go through a nation-wide shut-down because they were so quick to do extensive testing to identify those individuals who needed to be sequestered, but this isn’t the case with many other countries like the U.S. If Americans did not lock-down, but rather continued business-as-usual too soon, the nation could get to “herd immunity” (which requires about a 50% infection rate, or over 150,000,000 people), but it would devastate the health care system and cause many more deaths.
- Respiratory diseases are often seasonal, so there is a chance for lower infections as the weather warms. We’ll now this in a couple of months, given the experience of the Northern hemisphere (now getting warmer) and Southern hemisphere (now getting colder).
- If isolation is done well, within 20 days the infection numbers will change, particularly if there’s testing.
- There is some positive data on a few vaccines and drugs that have been put on a “therapeutic accelerator” to fast-track which of these should be prioritized for testing. Three or four may prove useful.
- People who recovered from COVID-19 have antibodies in their white immune cells. This is being examined as immune-booster, but this is hard to do and is difficult to scale to meet the need.
- Bill concludes with acknowledging that there are more pandemics to come, as I covered in Why Influenza and COVID-19 Pandemics Will Not Disappear, but hopefully when that happens we’ll be better prepared given what we’re going thorough now.
Now, let’s dig a bit deeper, aided by the fine work of the WHO, CDC, New York Times, Elisa Song, MD, James Robb, MD and Roger Seheult, MD.
What Is A Coronavirus?
It is a novel virus named for the crown-like spikes that protrude from its surface. The coronavirus can infect both animals and people. It can cause a range of respiratory illnesses from the common cold to more dangerous conditions like Severe Acute Respiratory Syndrome, or SARS.
The new coronavirus we’re concerned about is called COVID-19. It was first encountered in Wuhan, China, in December 2019, and has gone on to affect over 80,000 people around the globe, causing over 2,700 deaths so far. (Outdated info — check the stats at the beginning of this post and stay up to date with daily John Hopkins Situation Reports.) The virus can cause pneumonia. Those who have fallen ill are reported to suffer coughs, fever and breathing difficulties. In severe cases there can be organ failure. As this is viral pneumonia, antibiotics are of no use.
As of this original posting of this article in mid-March, the medical condenses is that the antiviral drugs we have against flu will not work. If people are admitted to hospital, they may get support for their lungs and other organs, as well as fluids. Recovery will depend on the strength of their immune system. Many of those who have died were already in poor health, and/or had unhealthy habits, such as smoking.
How Contagious Is This Coronavirus Outbreak?
According to preliminary research, it seems moderately infectious, similar to SARS, and is probably transmitted through sneezes, coughs and contaminated surfaces. That means, it spreads easily, which makes it hard to contain. Scientists have estimated that each infected person could spread it to somewhere between 1.5 and 3.5 people without effective containment measures, as compared to people with the seasonal flu who affect about 1.3 others on average.
To give you an idea about how the numbers play out:
-
- Seasonal flu infections after five cycles*: 5 people infect 45 others.
- COVID-19 infections after five cycles*: 5 people infect 365 others.
* The source of this information didn’t define “cycles”, but it might refer to the 2 to 14 day incubation period.
What Are The Symptoms Of COVID-19?
Many people who have COVID-19 have no symptoms, but from what I’ve been reading, the majority of infected people appear to have mild infections with mild cold-like symptoms and fever. Reported symptoms include:
-
- Fever (which may not be present in the very young or very old, or immunocompromised)
-
- Uncomplicated upper respiratory symptoms (Cough, sore throat, nasal congestion, malaise, headache, muscle aches)
-
- Difficulty breathing
-
- Mild pneumonia
-
- Severe pneumonia (the severe pneumonia caused by COVID-19 is now named severe acute respiratory infection (SARI))
-
- Acute Respiratory Distress Syndrome (ARDS)
-
- Sepsis and Septic shock
What’s Going On With Testing?
In a word — not enough!
Because of the urgent need for testing in the USA, the Food and Drug Administration (FDA) has allowed about 90 companies, many in China, to sell antibody tests designed to indicate whether people may have built immunity to the coronavirus.
The FDA has since warned that some of those businesses are making false claims about their products, and health officials in the U.S. and abroad have found other tests to be deeply flawed. Officials fear a repeat of the earlier launch of Covid-19 diagnostic tests that failed to monitor which Americans, and how many, had been infected.
Governors said on April 19 that a shortage of coronavirus tests was among the most significant hurdles to lifting restrictions in their states, in some cases rejecting the Trump administration’s assertions that the supply was adequate.
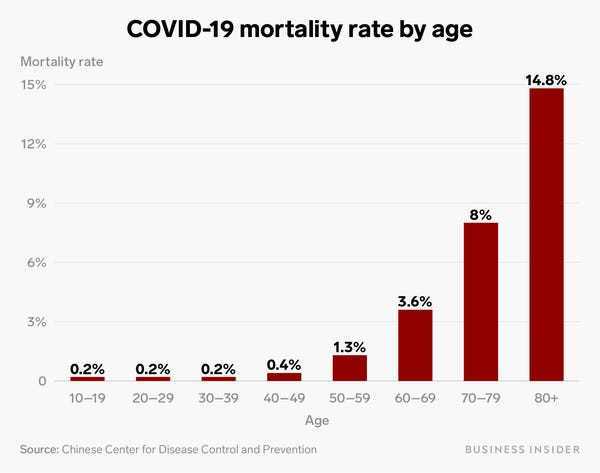
What is the COVID-19 mortality rates?
The mortality rate for COVID-19 has yet to be established. Those infected in China had a high mortality rate, but might have been an outlier given the lack of hospital staff, medical supplies, ICU beds, and test kits that China is was facing, as well as a higher percent of smokers that in many industrialized nations.
What we know so far:
-
- The most predictive factor is age — The older you are, the higher the chance for an unhappy outcome relative to younger folks. In a report released by the Chinese CCDC on February 17, 2020 in the Chinese Journal of Epidemiology, the risk of death increases with age, with being over 80 the highest risk factor. The fatality rate of patients over 80 years old was estimated to be 14.8%. Death in those under 50 appears to be unlikely, with the mortality rate of 40-49 year olds estimated to be 0.4% and 0.2% for patients 10-39 years of age.
-
- Children appear relatively spared —
There have been NO deaths in children 0-9 years old.Sadly, now there have been, and for some kids, it’s been due to preexisting health issues, such as obesity. (Read my article, Are COVID-19 and Obesity Linked?)
- Children appear relatively spared —
-
- Having a chronic, preexisting medical condition also significantly increased the risk of death. Without any pre-existing condition, the mortality rate was 0.9%. A history of cardiovascular disease increased the risk to 10.5%. [2]
-
- In China, males died at a higher rate from COVID-19 than females, but that might be because smoke more males smoke than females.
COVID-19 Prevention: Basic Tactics
The most important thing you can do to avoid getting infected during the coronavirus outbreak is to avoid crowds Then, there’s a few other basic preventive measures to take that I’ve gleaned from various news stories, Dr. Peter Attia, and Dr. James Robb, former professor of pathology at the University of California San Diego.
-
- Stay home
if you’re sickperiod.
- Stay home
-
- Scrub your hands frequently and thoroughly for at least 20 seconds and/or use a greater than 60% alcohol-based hand sanitizer whenever you return home from ANY activity that involves locations where other people have been.
-
- Keep a bottle of sanitizer available at each of your home’s entrances. AND in your car for use after getting gas or touching other contaminated objects when you can’t immediately wash your hands.
-
- Use disinfectant wipes at the stores when they are available, including wiping the handle and child seat in grocery carts.
-
- Amazon! Many of us will be using Amazon for deliveries of stuff we want instead of driving somewhere to get it. As Peter Attia MD advises: Open the package outside, wipe down whatever you bought with a disinfectant once inside, and then thoroughly wash your hands for 20 seconds or more.
-
- Stay more than six feet (two meters) away from sneezing, coughing people
-
- Don’t shake hands or put your face/lips next to another person’s face/lips unless you’re certain they’re not infected, which by the way you won’t know during the first seven to 14 days a person is infected, because during that period they may not show symptoms.
-
- If possible, cough or sneeze into a disposable tissue and discard. Use your elbow only if you have to. The clothing on your elbow will contain infectious virus that can be passed on for up to a week or more!
-
- Use ONLY your knuckle to touch light switches. elevator buttons, etc.. Lift the gasoline dispenser with a paper towel or use a disposable glove.
-
- Open doors with your closed fist or hip – do not grasp the handle with your hand, unless there is no other way to open the door. Especially important on bathroom and post office/commercial doors.
-
- Keep a 30-day supply of essential medicines and household items.
-
- Get a flu shot — it might not help with COVIDS-19, but could protect against the seasonal flu and thereby prevent that from complicating matters.
-
- Only use surgical masks if you can’t resist touching your face (mouth and eyes), given that this is a common way of getting infected. The mask will help prevent your hands from touching much of your face, and keep you from infecting others, should you be infected, but does little to protect you from infection, say health experts.
-
- Consider using zinc lozenges. Dr. Robb says they are effective in blocking coronavirus (and most other viruses) from multiplying in your throat and nasopharynx. Use as directed several times each day when you begin to feel ANY “cold-like” symptoms beginning. It’s best to lie down and let the lozenge dissolve in the back of your throat and nasopharynx. Cold-Eeze lozenges is one brand available, but there are other brands available, such as Zicam Cold Remedy, which has has a 4.7 rating on Amazon.com
COVID-19 Prevention: Better Tactics
In addition to doing the Basic Tactics:
-
- Supply yourself with foods and spices with antiviral properties — These include coconut oil, raw garlic, oregano, ginger, kimchi and other fermented foods, walnut, pomegranate, green tea, apple cider vinegar, and medicinal mushrooms (shiitake, maitake, reishi, cordyceps, turkeytail).
-
- Eat colorful fruits and vegetables — They’re full of antioxidants which will help destroy the free radicals that weaken your immune system. If you rather die from coronavirus than eat an veggie, try adding them to a smoothie, along with some hemp, pea or whey protein powder.
-
- Drink bone broth — Bone broth has amazing immune-supporting properties, and with this recipe you can make your own.
-
- Eat fermented foods — The probiotics contained in fermented foods have immune boosting powers. In fact, the fermented Korean cabbage, kimchi, was found to have significant effects in preventing and fighting the H1N1 influenza virus! Other examples of delicious fermented foods to try include sauerkraut, pickles (try “real” pickles without added vinegar like Bubbies), miso, kefir, and kombucha.
-
- Avoid simple sugars and processed junk food — So pernicious are that your immune system is compromised within 30 minutes of eating simple sugars, like glucose, refined sugar, and fructose. Such foods can also cause a 50% reduction in your white blood cells’ abilities to kill germs. White blood cells is the “army” that fight off germs. This effect is most noticeable two hours after ingestion, but is still present five hours later. Keeping blood sugar levels healthy has been shown to improve immune system activity.
-
- Get fresh air and moderate daily exercise — Moderate exercise can boost the production of macrophages, the kind of white blood cells that “eat” bacteria and viruses. However, intense exercise can actually temporarily decrease immune function – so don’t overdo it! (Read my article, Short Home Workouts You Can Do Now With Surprising Results.)
-
- Get adequate sleep — An increase in sleep actually increases the number of your white blood cells. On the other hand, loss of sleep even for a few hours at night, increases inflammation in our body which makes us more susceptible to catching the flu and having more severe symptoms. Try melatonin.
-
- Reduce the stress — Emotional stress creates physiological stress in our bodies that lowers our immune defenses and makes us more vulnerable to illness. Stress has been shown to lower our white blood cells’ abilities to kill germs, and actually creates more inflammation that may make us feel even sicker. (For guidance on how to help manage stress, read my article, Why Chronic Stress Is The Biggest Super-Ager Of Them All.)
COVID-19 Prevention: Best Tactics
Click here for more immune boosting tips, with a more extensive list of medicinal mushrooms.
In addition to doing the Better Tactics:
Irrigate your nose
While we do not know if nasal irrigation makes a difference for prevention of
COVID-19, a major preventive thing you can do for any viral respiratory illness is to irrigate your nasal passages with Xlear nasal spray at the end of every day, and after any exposure to crowds (work, school, playgroups, plane travel, etc.). This is a saline nasal spray with xylitol and grapefruit seed extract, both of which have antimicrobial properties. This is one of the MOST important things that we can do to prevent influenza and other viral respiratory infections from taking hold, says Dr. Elisa Song, because after exposure to it, the influenza virus tries to invade and multiply in your nasal passages for at least one to two days before you develop symptoms. Nasal irrigation can wash away viral particles before they have the opportunity to take hold, and thereby prevent many infections from occurring.
Coat your throat
Take a zinc lozenge or spray.
Take your vitamins
- Fish oil – Long-chain omega-3 fatty acids like fish oil may help boost the immune system by enhancing the function of immune cells. [3]
- Vitamin C – Vitamin C is a powerful antioxidant which assists our ability to ward off and deal with infection. Consider using Metagenics Ultra-Potent C because it has added ingredients such as lysine and glutathione which assist in fighting viruses.
- Vitamin D3 – There is speculation that rates of illness increase over the winter because of the widespread deficiency of Vitamin D. As mentioned above, Vitamin D deficiency may be one of the risk factors for sepsis. Studies have shown that people supplemented with adequate levels of Vitamin D3 during the cold and flu season had significantly lower rates of infection. Vitamin D3 increases our body’s production of cathelicidin, an antimicrobial compound, to help fight viral and bacterial infections. The Vitamin D Council recommends a maintenance dosage of 1000IU of Vitamin D3 per 25 pounds of body weight (the dosage may be higher in people with Vitamin D deficiency, which is epidemic and can be measured through an easy blood test).
- Zinc – Zinc is required for the normal functioning of white blood cells. Supplementing with just 15mg of zinc per day in adults has been found to improve our immune cells’ ability to ward off infection.
Take some shrooms
My Community and Mycoshield, both from Host Defense, offer more than a dozen mushroom extracts, grown and prepared by one of most revered mycologists in the world, Paul Stamets, PhD.
Make your own Anti-flu Supertonic
You’ll need horseradish root, garlic, onion, ginger root, jalapeño pepper and apple cider vinegar. Here’s how to make it.
Read my articles about how to prevent influenza, as they have plenty of more suggestions.
Should You Wear A Mask?

Yours truly in a purposely silly get-up, but that face “mask” I’m wearing is the simplest thing you can wear that’s somewhat protective. I’m wearing a folded-over balaclava, but a scarf will do.
Update:
There are many instructinal videos on YouTube about how to make a cloth facemask. Frankly, most require more “tools” or sewing skill than many will muster together, so I selected a technique that’s both simple and effective to share with you, thanks to Raphaela Laurean:
Face masks are currently not recommended for the general public during the coronavirus outbreak, mainly because the good ones aren’t available, there can be a problem with fit and a problem with how we use them. Face masks are only recommended if you have a cough that you could transmit, or are taking care of someone who is sick with COVID-19. They are also helpful to prevent you from touching your face, although rubbing your eyes is another matter, which you should avoid.
But if you do wear a face mask, make sure it’s a “Particulate Respirator Mask” that filters at least 95% of very small particles and is marked P95, R95 or N95, has 2 straps, and forms a tight seal around your nose and mouth, says Dr. Song. A regular surgical mask will provide no protection and is actually meant to protect others from your cough or sneeze.
A properly fitted respirator mask should be worn over BOTH the nose and mouth, and form a tight seal so that you can’t smell any ambient odors. A good test is to put on the mask covering your mouth and nose, pinch the mask across the bridge of your nose, then spray peppermint or lavender essential oil in front of your face. You should not be able to smell or taste any of the oil in your nose or mouth through the mask.
Your Takeaway
Be safe, rather than sorry. Yes, if you’re healthy and get infected with COVID-19, as it now appears, you’ll recover. But why go through that drama! While the cornoavirus outbreak is still underway, take the precautionary measures listed above.
At minimum, I encourage you to:
- Stay away from crowds.
- Wash your hands regularly.
- Supplement with some immune-enhancers.
- Use Xlear nasal spray at the end of every day should people in your area become infected.
- It might be a good idea to try some zinc supplementation, particularly a lozenge or spray.
Last Updated on February 7, 2024 by Joe Garma