Avoid Getting Osteoarthritis As You Age

Avoid getting osteoarthritis as you get older by developing a strategy now. Choose from this large list of things to do that can relieve some of the pain and discomfort you may be feeling now, or to help prevent ever becoming compromised by arthritis.
How can we avoid getting osteoarthritis as we grow older?
That’s the question a recent New York Times article posed to exercise physiologist Kelli Dominick Allen, and geriatrician Wayne McCormick. The answers aren’t absolute, but multi-layered, consisting of best practices along the lines of nutrition, exercise, preventative care, herbs, supplements and assistance from health professionals.
All that sounds reasonable, but, frankly, trite. What you need are some details, and they’re coming.
In this post, I’m going to expand upon the observations made in the NYTimes article, to include:
- Why osteoarthritis is not inevitable as you age
- How osteoarthritis happens
- How to avoid getting osteoarthritis (or treat it)
- Can herbs and supplements help relieve osteoarthritis?
- Eat these foods to improve osteoarthritis and grow cartilage
The aim here is to give you a roadmap to avoid getting osteoarthritis as you get older, or if you already are grappling with it, to help you reduce the symptoms and pain.
Let’s dig in…
Why osteoarthritis is not inevitable as you age
A lot has to happen if you don’t want to age like most everybody else. If you want to be able to jog, play tennis or lift weights without feeling sore in your shoulder, hip, knee or ankle joints for days afterwards, you’ve got to have a strategy to avoid getting arthritis.
In a recent survey conducted in the United States, encompassing more than 2,200 individuals aged between 50 and 80, 60 percent disclosed that they had arthritis. Moreover, about three-quarters of respondents regarded joint pain and arthritis as inherent aspects of the aging process.
Nonetheless, the progression towards arthritis is not a foregone conclusion as we age. Dr. Kelli Dominick Allen, an exercise physiologist at the University of North Carolina School of Medicine, asserts that thinking about arthritis as an unavoidable fate due to aging is incorrect [1].
Arthritis is an umbrella term encompassing over 100 types of inflammatory joint conditions, each arising from various causes. Many of these causes have limited connections to age, according to Dr. Allen.
However, there is one type of degenerative joint ailment, osteoarthritis, that does become somewhat more likely as individuals grow older. This condition, often attributed to worn-out joints, is most frequently observed among individuals over 50, particularly women, notes Dr. Wayne McCormick, a geriatrician at the University of Washington School of Medicine [1].
It’s important to distinguish between osteoarthritis and rheumatoid arthritis in order to determine the proper treatment. They are very different.
Here are the differences between the two:
Osteoarthritis:
- Most common form of arthritis
- Caused by mechanical wear and tear on joints
- Occurs when the smooth cartilage joint surface wears out
- Usually begins in an isolated joint
- Affects weight-bearing joints such as the knees, hips, and feet
- Symptoms include pain, stiffness, and limited movement in the affected joint
- Cartilage breakdown, inflammation, and bone changes are the main factors that contribute to the development of osteoarthritis
- Most common form of arthritis that occurs as we get older
Rheumatoid arthritis:
- An autoimmune disease in which the body’s own immune system attacks the body’s joints
- Causes pain, swelling, and stiffness in the joints
- Often targets several joints at one time
- Symptoms include joint pain, swelling, stiffness, and fatigue
- Can affect people of any age, but usually begins between the ages of 30 and 50
- Cartilage breakdown, inflammation, and bone changes are also factors that contribute to the development of rheumatoid arthritis
The exact reasons behind why some people experience more joint inflammation and pain with age than others remain uncertain. What is known is that:
- Around 12 percent of osteoarthritis cases can be traced back to joint injuries sustained during youth, such as meniscus or ligament tears [2].
- Family history plays a part — osteoarthritis is more prevalent among those who had or have family members with the condition.
- Osteoarthritis is more prevalent in individuals managing chronic health issues such as obesity, heart disease, or diabetes.
Osteoarthritis can affect any joint in the body, but it most commonly affects the following joints:
- Hands: osteoarthritis can affect the joints in the fingers, thumbs, and wrists[3][4][5].
- Knees: osteoarthritis of the knee, also known as gonarthrosis, is the most common location of osteoarthritis. It most often affects women after the age of 40 [5][6].
- Hips: osteoarthritis of the hip is another common location of osteoarthritis, particularly in older adults [3][4][5][7].
- Spine: osteoarthritis can affect the joints in the spine, particularly in the neck and lower back [3][4][5].
- Feet: osteoarthritis can affect the joints in the feet, particularly the big toe [4][8].
- Weight-bearing joints: osteoarthritis can affect any weight-bearing joint, such as the knees, hips, and feet, due to the increased stress on these joints [4][7]
It’s important to note that while osteoarthritis can affect any joint, some joints are more commonly affected than others [4][5].
Citations
Citations:
[3] https://myhealth.alberta.ca/Health/Pages/conditions.aspx?hwid=zm249 [4] https://www.nia.nih.gov/health/osteoarthritis [5] https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925 [6] https://www.arthrolink.com/en/disease/knowing/joints-involved [7] https://www.arthritis.org/diseases/osteoarthritis [8] https://versusarthritis.org/about-arthritis/conditions/osteoarthritis/
How osteoarthritis happens
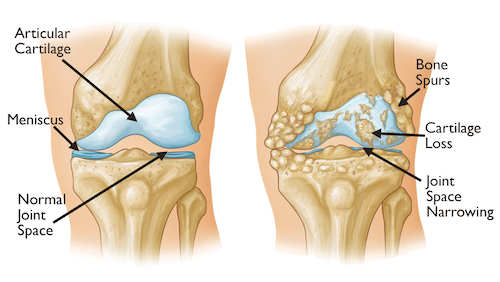 Osteoarthritis develops in the joints due to the following factors:
Osteoarthritis develops in the joints due to the following factors:
- Cartilage breakdown: osteoarthritis occurs when the cartilage that cushions the ends of bones in the joints gradually deteriorates. Cartilage is a firm, slippery tissue that enables smooth joint motion [9].
- Changes in cartilage: with osteoarthritis, part of the cartilage thins and the surface becomes rougher, leading to decreased joint mobility and increased friction between bones [10].
- Bone changes: osteoarthritis affects the entire joint, including the bone. It can cause changes in the bone structure, such as the development of bone spurs or osteophytes, which can further contribute to joint pain and limited mobility [11].
- Connective tissue deterioration: osteoarthritis also affects the connective tissues that hold the joint together and attach muscles to bones. These tissues can deteriorate, leading to joint instability and inflammation [9].
- Inflammation: osteoarthritis can cause inflammation of the joint lining, leading to pain, swelling, and further damage to the joint [9].
Several factors can increase the risk of developing osteoarthritis, including joint injuries or overuse, obesity, musculoskeletal abnormalities, and genetic predisposition [11][12].
While the exact mechanisms of cartilage loss and bone changes in osteoarthritis are not fully understood, ongoing research aims to better understand the disease and develop effective treatments, including cartilage regeneration techniques [13].
Citations
Citations:
[9] https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925 [10] https://versusarthritis.org/about-arthritis/conditions/osteoarthritis/ [11] https://www.arthritis.org/diseases/osteoarthritis [12] https://my.clevelandclinic.org/health/diseases/5599-osteoarthritis [13] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4426098/
Dr. Allen, the exercise physiologist, suggests that the process of preventing osteoarthritis later in life should commence years before it becomes a concern. This involves taking precautions to prevent joint injuries during physical activities and sports, coupled with proper recovery when such injuries do occur.
For individuals not at risk of sports-related injuries, remaining physically active and managing a healthy weight can aid in curbing excessive joint wear and tear, potentially reducing pain should osteoarthritis manifest in later years.
A review of 44 clinical trials conducted in 2015 revealed that regular exercise resulted in diminished knee pain related to osteoarthritis, along with improved physical function and quality of life.
Low-impact exercises like stationary cycling, which minimize impact on knees, hips, and joints, are particularly beneficial. Strengthening muscles such as the quadriceps and hamstrings provides joint support, according to geriatrician Dr. McCormick.
In addition to regular exercise, various measures such as supportive knee or ankle braces, over-the-counter pain relievers like ibuprofen or acetaminophen, and steroid injections into problematic joints can offer varying degrees of joint pain relief.
Certain dietary supplements like glucosamine and chondroitin sulfate, as well as herbal remedies like Boswellia, are believed to alleviate symptoms for some individuals. Yet, scientific support for their use remains limited. Nevertheless, Dr. McCormick suggests that these supplements are unlikely to be harmful, making them worth considering—either to try or discontinue if they prove ineffective. (I’ll tell you about some supplements you might consider below.)
Ultimately, the key to diminishing the risk of developing osteoarthritis as we age is to adopt a lifestyle that is pain-free, active, and health-conscious. Dr. Allen asserts that many of the strategies proven effective in reducing the risk of chronic conditions like diabetes or heart disease are also powerful tools for mitigating age-related joint issues. She says:
Someone striving for a healthy lifestyle will already be implementing the most crucial measures for lowering the risk of osteoarthritis
Kelli Dominick Allen
How to avoid getting osteoarthritis (or treat it).
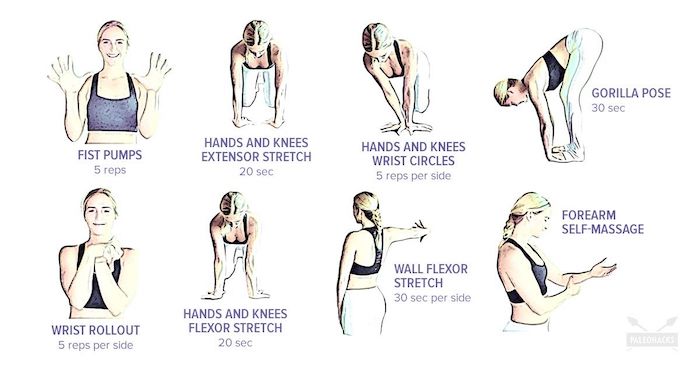
These stretches are for the wrist, but there are many that can be done for every joint. (Click image to enlarge)
Watch the mobility videos I curated from YouTube
What follows is a rundown of the various ways you could avoid getting osteoarthritis or treat it should it already be a forgone conclusion.
- Maintain a healthy weight: being overweight puts extra stress on your joints, which can increase the risk of developing osteoarthritis [14][15][16]. What’s a “healthy weight”? Check your waist-to-height ratio.
- Exercise regularly: regular exercise can help to prevent joint injuries during sports or exercise, and help you recover properly when they occur. It can also help to prevent excessive wear and tear of your joints and reduce pain if osteoarthritis sets in later in life [14][15]. Here are my posts about exercise.
- Protect your joints: avoiding joint injuries is key to preventing osteoarthritis. This includes using proper form during exercise, wearing protective gear when playing sports, and making sure your workplace is safe and free of fall hazards [15].
- Control your blood sugar: people with diabetes are more likely to develop osteoarthritis, so it’s important to manage your blood sugar levels [16]. Here are my posts about controlling blood sugar.
- Eat a healthy diet: eating a diet that’s low in sugar, alcohol, and processed foods can help to reduce inflammation in the body, which can contribute to osteoarthritis [14]. Eat like a gorilla, or a Blue Zoner.
- Quit smoking: smoking can increase the risk of developing rheumatoid osteoarthritis, so quitting smoking can help to reduce this risk [15].
- Consider supplements and herbs: while there isn’t much scientific evidence to support their use, some herbs and supplements, such as turmeric, ginger, and glucosamine/chondroitin and Boswellia have anti-inflammatory properties and may help reduce pain and inflammation associated with osteoarthritis. [17][18]. (More on this topic below.)
- Medications: over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) such as aspirin, ibuprofen, and naproxen can help reduce pain and inflammation associated with osteoarthritis [19][20][21]. Acetaminophen (Tylenol) may also be used to relieve pain, although it does not have anti-inflammatory properties [20].
- Physical therapy: physical therapy can help improve joint function, reduce pain, and increase strength and flexibility. A physical therapist can provide exercises and techniques tailored to the individual’s specific needs [20].
- Assistive devices: the use of assistive devices such as braces, splints, or canes can help support and stabilize the affected joints, reducing pain and improving mobility [22][23].
- Heat and cold therapy: applying heat or cold to the affected joints can help alleviate pain and reduce inflammation. Heat therapy, such as warm showers or heating pads, can help relax muscles and improve blood circulation. Cold therapy, such as ice packs, can help numb the area and reduce swelling [20].
- Complementary and alternative therapies: some people find relief from osteoarthritis symptoms through complementary and alternative therapies such as acupuncture, massage, or transcutaneous electrical nerve stimulation (TENS) [20].
- Surgery: in severe cases where conservative treatments are not effective, surgical options such as joint replacement or joint fusion may be considered. These procedures aim to relieve pain and improve joint function[ 24].
- Acupuncture: acupuncture involves the insertion of thin needles into specific points on the body to stimulate the body’s natural healing processes. Some studies have suggested that acupuncture may help reduce pain and improve joint function in people with osteoarthritis[25][26].
- Massage: massage therapy can help reduce muscle tension and improve circulation, which can help alleviate pain and stiffness associated with osteoarthritis [26].
- Chiropractic: chiropractic adjustments can help improve joint function and reduce pain associated with osteoarthritis. However, it’s important to consult with a healthcare professional before seeking chiropractic treatment [26].
Citations
Citations:
[14] https://www.arthritis.org/health-wellness/about-arthritis/understanding-arthritis/reduce-your-risk [15] https://www.healthline.com/health/arthritis-prevention [16] https://jerseyrehab.com/tips-to-prevent-arthritis-in-elderly-patients/ [17] https://www.aafp.org/pubs/afp/issues/2003/0115/p339.html, [18] https://www.healthline.com/health/osteoarthritis-alternative-treatment [19] https://www.webmd.com/arthritis/options-basics [20] https://www.mayoclinic.org/diseases-conditions/osteoarthritis/diagnosis-treatment/drc-20351930 [21] https://www.webmd.com/osteoarthritis/medicines-treat-oa [22] https://www.healthline.com/health/osteoarthritis/over-counter-relief [23] https://www.arthritis.org/health-wellness/treatment/complementary-therapies/supplements-and-vitamins/12-supplements-for-osteoarthritis [24] https://www.arthritis.org/diseases/osteoarthritis [25] https://www.aafp.org/pubs/afp/issues/2003/0115/p339.html [26] https://www.webmd.com/osteoarthritis/features/alternative-arthritis-treatments
Let’s expand on the use of herbs and supplements.
Can herbs and supplements help relieve osteoarthritis?
There are some over-the-counter compounds that may help alleviate arthritis symptoms or promote cartilage growth. However, it’s important to note that the effectiveness of these compounds may vary, and it’s always best to consult with a healthcare professional before starting any new supplements or medications.
I’ve already touched on some of these, but here’s a bit more about them, as well as a few more to consider:
- Glucosamine and chondroitin: these supplements are commonly used for arthritis and are components of cartilage, which cushions the joints. They may help control pain, but they do not seem to help the joint grow new cartilage or prevent arthritis from getting worse [27][28].
- SAM-e: S-adenosylmethionine (SAM-e) is an over-the-counter supplement that acts as an analgesic or pain reliever and has anti-inflammatory properties. It may stimulate cartilage growth and help alleviate arthritis pain [29].
- Boswellia serrata: also known as Indian frankincense, Boswellia serrata is a supplement that has shown promise for osteoarthritis. It may help reduce inflammation and alleviate arthritis symptoms [29].
- Curcumin: curcumin supplements have anti-inflammatory properties and may help reduce arthritis pain, particularly in osteoarthritis [29].
- Fish oil: fish oil supplements, which contain omega-3 fatty acids EPA and DHA, have anti-inflammatory properties and may help reduce arthritis symptoms, particularly in rheumatoid arthritis [29][30].
- Avocado-soybean unsaponifiables (ASU): ASU is a supplement derived from avocado and soybean oils. It may help reduce inflammation and slow down the progression of osteoarthritis [29].
- Ginger: ginger supplements have anti-inflammatory properties and may help alleviate arthritis pain, both in rheumatoid arthritis and osteoarthritis [29].
Citations
Citations:
[27] https://www.arthritis.org/health-wellness/treatment/complementary-therapies/supplements-and-vitamins/vitamins-supplements-arthritis [28] https://www.mountsinai.org/health-library/selfcare-instructions/medicines-injections-and-supplements-for-arthritis [29] https://www.arthritis.org/health-wellness/treatment/complementary-therapies/supplements-and-vitamins/supplements-for-arthritis [30] https://www.webmd.com/osteoarthritis/medicines-treat-oa
Of course, what you eat is important too.
Eat these foods to improve osteoarthritis and grow cartilage
Here are some foods that can help improve osteoarthritis and grow cartilage:
- Dairy: dairy products, especially yogurt, are a good source of calcium and vitamin D, which are important for bone health and cartilage growth, but I wouldn’t go too heavy on this, as there’s some debate that dairy products might be inflammatory [33][34][35][36][37][38].
- Brown rice: brown rice is a great source of hyaluronic acid, which is essential for protecting and rebuilding cartilage [39][31].
Bone broth: bone broth is packed full of collagen and proteins that are perfect for joint health [31]. - Blueberries: blueberries are rich in antioxidants, which can help reduce inflammation and protect against cartilage damage [39][31].
- Fish: oily fish such as salmon, mackerel, and sardines are rich in omega-3 fatty acids, which have anti-inflammatory properties and can help reduce joint pain and stiffness [31][32].
- Oranges: oranges are a good source of vitamin C, which is important for collagen production and cellular healing. Vitamin C can also promote cartilage regeneration and protection [40]. Note: oranges, NOT orange juice, which has too much sugar and not enough fiber.
- Leafy greens: leafy greens such as kale, spinach, and collard greens are rich in antioxidants, which can help protect against cartilage damage [41].
- Broccoli: broccoli contains a compound called sulforaphane, which researchers believe could slow the progression of osteoarthritis. It is also rich in vitamins K and C, as well as calcium, which helps strengthen bones [42][32].
It’s important to note that while these foods can help improve osteoarthritis and promote cartilage growth, they should be consumed as part of a balanced and nutritious diet. See my posts about diet and nutrition.
Citations
Citations:
[33] https://www.usdairy.com/news-articles/dairy-and-inflammation [34] https://pubmed.ncbi.nlm.nih.gov/26287637/ [35] https://www.cleaneatingmag.com/clean-diet/general-health/whats-the-deal-with-dairy-and-inflammation/ [36] https://www.eatingwell.com/article/2056066/heres-what-a-dietitian-says-about-dairy-causing-inflammation/ [37] https://www.healthline.com/nutrition/is-dairy-inflammatory [38] https://www.arthritis.org/health-wellness/healthy-living/nutrition/healthy-eating/dairy-and-inflammation [39] https://www.mobilitypluscolorado.com/blog/increase-cartilage-in-joints-naturally [40] https://arrowheadhealth.com/foods-that-help-rebuild-cartilage/ [31] https://mobilitydeck.com/foods-for-rebuilding-cartilage/ [41] https://www.drpatelchirag.com/blog/food-for-healthy-joints-and-cartilage/ [42] https://www.vinmec.com/en/news/health-news/nutrition/good-foods-for-joint-cartilage/ [32] https://www.medicalnewstoday.com/articles/322603
Well, now you have quite a bit to chew on. If you’d like to read more about arthrits, check out my three-part series (so far):
How You Can Beat Arthritis, Part 1
How You Can Beat Neck Arthritis, Part 2
How You Can Beat Shoulder Arthritis, Part 3
Last Updated on February 25, 2024 by Joe Garma






