Diet Misinformation, Keto and the Med

Diet misinformation is everywhere. If you don’t want to be led down the wrong path, you need to pay attention to the authority of the writers, researchers, institutions and, yes, YouTubers. Here I’m added by some experts to reveal some common nutrition misinformation, and delve into the science behind fats and carbs as they relate to weight loss, as well as the big reveal — the Med.
Diet misinformation has become a significant problem in modern society. The rise of the internet and social media has made it easy for anyone to share their opinion on nutrition, regardless of their qualifications or level of expertise. As a result, many people are confused about what to eat, how much to eat, and what is healthy. This confusion can lead to poor dietary choices and negative health outcomes.
Content: Diet Misinformation Sugar is toxic? Is a low-carb/high-fat diet best? Is coffee good or bad? Contradict diet misinformation CICO vs CI The CICO/CI obesity tussle The Rogan-led debate and Norton Critique The problems with Keto What is the Keto Diet? Is Keto good for fat loss? More problems with Keto Diet Misinformation Go Mediterranean! What is the Med Diet and what is it good for? Med Diet's cellular effects revealed Start eating Mediterranean
Let’s dig in…
Diet Misinformation Abounds
Stephan Guyenet wrote an article entitled Read This, Not That: The Hidden Cost of Nutrition Misinformation to highlight the dangers of nutrition misinformation and provide examples of how it can be harmful.
Dr. Guyenet is a neurobiologist and obesity researcher. In his article, he emphasizes the importance of evidence-based nutrition, and the dangers of relying on fads or unproven theories.
Sugar Is Toxic?
One example Dr. Guyenet provides is the idea that sugar is toxic and should be avoided at all costs. He points out that while excess sugar intake can be harmful, the evidence does not support the idea that sugar is toxic. We’re talking real sugar here, not Aspartame (NutraSweet, Equal), Saccharin (Sweet’N Low), or Sucralose (Splenda).
The human body is capable of processing and utilizing sugar in moderation without negative health effects. According to the American Heart Association:
- Men should consume no more than 9 teaspoons (36 grams or 150 calories) of added sugar per day (check food labels).
- Women should limit their consumption to 6 teaspoons (25 grams or 100 calories) per day (check food labels).
Keep in mind that one 12-ounce can of soda contains 8 teaspoons (32 grams) of added sugar! (Read my post, 1 Soda, 60 Minutes of Hell.)
The demonization of sugar has led to the rise of alternative sweeteners, such as stevia and monk fruit, which are marketed as healthier alternatives. However, these sweeteners have not been studied extensively, and their long-term health effects are not well understood. Nonetheless, if your sweet tooth can’t be denied, try substituting them for regular sugar, and certainly for Aspartame, Saccharin and Sucralose.
Is A Low-carb/High-fat Diet Best?
Another example Guyenet provides is the promotion of a low-carb, high-fat diet for weight loss. While this diet can be effective for some people, he argues that it’s not a one-size-fits-all solution. The human body is complex, and different people may respond differently to different diets. Additionally, a high-fat diet can be difficult to sustain long-term and can lead to nutrient deficiencies if not carefully planned. Guyenet stresses the importance of individualized nutrition advice based on a person’s unique needs and preferences.
Is Coffee Good or Bad?
Read my post, Does Drinking 2 Cups of Coffee Improve Health and Longevity?
In September 2022, The European Journal of Preventive Cardiology published a 2022 study that said British adults who drink two to three cups of coffee per day are at a lower risk of developing cardiovascular disease and dying than those who don’t drink coffee.
Doesn’t this suggest that coffee is good for the heart and keeps us from dying?
The problem is that this is an observational study, which means there were no controls; hence, it’s not clear that the association is due to the coffee itself, rather than some other difference between people who drink a lot of coffee versus people who don’t. I mean, it could be that British people who don’t drink coffee drink whiskey instead. Yes, that’s a silly notion, but I want to emphasize that observational studies spark more questions than they answer.
When a study is not a double-blind, placebo study, interpretations can get out of hand. For instance, as Guyenet describes, although the authors of the paper are fairly cautious in their interpretation (they describe the finding as an association and only obliquely imply that drinking coffee reduces health risks), once the media gets a hold of it, “the shackles of restraint have been cast off”. For instance, a CNN Health article headline shouts, Coffee lowers risk of heart problems and early death. Then the article presents two sentences admitting that the findings don’t necessarily imply cause and effect, then proceeds as if they do.
Diet Misinformation Needs To Be Contradicted
Guyenet goes on to cite some ridiculous claims rife with diet misinformation. For instance, did you know that:
- The scent of vanilla increases blood flow to the penis?
- People with Type B blood can eat all types of dairy and remain in good health?
- Eating too little salt as a child increases a person’s risk of drug addiction later in life?
These questionable claims abound in popular nutrition books. You may chortle at such claims, but it’s no laughing matter that Americans buy about 5 million diet books per year, many of them soaked in diet misinformation.
Dr. Guyenet’s article serves as a reminder of the importance of evidence-based nutrition and the dangers of relying on fads or unproven theories. Nutrition is a complex field, and individualized advice based on a person’s unique needs and preferences is essential for optimal health outcomes.
It’s also important to be critical of nutrition information found on the internet and social media, as many sources may not be credible or trustworthy. This includes me. I endeavor to use credible sources of information, and never aim to misinform, but my interpretations of scientific studies can be wrong, and new studies can often contradict older ones; this the very basis of scientific discovery.
Speaking of science, what does it say about the best diet for weight loss?
Well, here too, confusion abounds.
CICO vs CI
What causes obesity, and what are the mechanisms behind weight loss?
There are lots of explanations and assertions on those topics, none more prominent than the Calories In/Calories Out (CICO) model versus the Carbohydrate-Insulin (CI) model. While both models have been extensively studied, there is significant debate over their relative scientific rigor.
Let’s start off by comparing and contrasting the scientific rigor of these two models, and then weigh in on a debate that podcaster Joe Rogan hosted between a defender of CI, Gary Taubes, (sss) and a defender of CICO, your now familiar Dr. Stephan Guyenet, as seen through the lens Dr. Layne Norton.
The CICO/CI Obesity Tussle
The CICO model proposes that weight gain occurs when caloric intake exceeds caloric expenditure, while weight loss occurs when caloric intake is less than caloric expenditure. This model is based on the first law of thermodynamics, which states that energy cannot be created or destroyed, only converted from one form to another. Therefore, according to this model, any excess energy consumed that is not burned will be stored as fat.
The CI model, on the other hand, proposes that weight gain occurs when there is an excessive secretion of insulin in response to carbohydrate-rich foods. According to this model, high levels of insulin cause the body to store more energy as fat, leading to weight gain. Conversely, reducing carbohydrate intake reduces insulin secretion and promotes fat burning, leading to weight loss.
What it comes down to is that some studies have suggested that both types of diets can lead to weight loss when calorie intake is controlled, others have shown differences in weight loss and metabolic effects between the two diets:
The question of whether high fat/low carb and low fat/high carb diets have the same impact on weight loss given equivalent calorie consumption is a subject of ongoing research and debate in the scientific community. While some studies have suggested that both types of diets can lead to weight loss when calorie intake is controlled, others have shown differences in weight loss and metabolic effects between the two diets.
Among the many, many such studies, here are three that represent the whole:
A 2014 study published in the Annals of Internal Medicine found that in overweight and obese adults, a low-carbohydrate diet resulted in significantly more weight loss than a low-fat diet over a 12-month period, even when calorie intake was similar between the two diets. However, the study also found that both diets resulted in significant weight loss and improvements in cardiovascular risk factors.
In contrast to the 2014 study, one published in 2018 in the Journal of the American Medical Association found the inverse was true — that over a 12-month period, a low-fat diet resulted in more body fat loss than a low-carbohydrate diet when calorie intake was similar between the two diets. Like the 2014 study, however, this one also found that both diets resulted in significant weight loss and improvements in metabolic risk factors.
And in 2022, a systematic review and meta-analysis of 33 studies involving a total of 3,939 participants concluded that “At 24 months, the effects on weight loss and improvement of metabolic risk factors were at least the same” between low-carbohydrate diets and low-fat diets.
So, at this point, the evidence suggests that:
Both high fat/low carb and low fat/high carb diets can lead to weight loss when calorie intake is the same, but there may be differences in weight loss and metabolic effects between the two diets that depend on factors such as the individual’s metabolism and health status.
I’ll explain more about how that happens.
The Rogan-led Debate and Layne Critique
OK, now that you’ve got a feel for the CICO vs CI debate, we can add some nuance to this argument (or complexity) by reviewing Dr. Laye Norton’s analysis of a Joe Rogan debate between Dr. Stephan Guyenet and Gary Taubes.
Joe Rogan is perhaps the most listened to podcaster in America, and he likes to “stir the pot”. In this case, the pot two primary ingredients, and one ancillary:
- Gary Taubes is a journalist and author who espouses the low carb/low insulin diet. He’s a debate participant and thereby a primary ingredient.
- Stephan Guyenet, PhD you already know from the “Diet Misinformation” section above. He debated Gary Taubes and is also a primary ingredient to the pot Joe Rogan stirred.
- Dr. Layne Norton holds a PhD in nutritional science, and is a powerlifting and coach. His analysis of the debate is what I’m about to review.
In his analysis of the debate, Dr. Norton first lays out the basic tenets of the CICO/CI debate; namely:
Argued by Taubes — The CI model that posits that insulin is the primary driver of obesity and that a high-carbohydrate diet leads to excess insulin secretion and subsequent weight gain through hormonal responses is correct. Taubes posits that reducing carbohydrate intake and increasing fat consumption can lead to weight loss.
Argued by Guyenet — While Insulin does play a role in weight regulation, it’s only one of many factors and that the overall energy balance equation (the CICO model) is the primary determinant of body weight. Guyenet argues that total caloric intake, rather than specific macronutrient composition, is the primary driver of weight gain. He suggests that reducing caloric intake and increasing physical activity are the most effective ways to promote weight loss.
They both present studies that back up their perspectives, although Taubes tends to dismiss the studies referred to by Guyenet without explanation; whereas Guyenet attempts to explain why Taubes cited studies are flawed, or have been superseded by more recent science.
Layne Norton is apoplectic that when asked if incontrovertible science proved that his position was wrong, would he capitulate, Taubes said no. That, Norton asserts, disqualifies him from scientific inquiry.
Overall, Norton argues that a more nuanced approach that considers the many factors that contribute to obesity is necessary for a comprehensive understanding of the condition.
Norton highlights several key points made by each participant in the debate. Taubes cites studies showing that low-carbohydrate diets lead to greater weight loss than low-fat diets, while Guyenet argues that these studies are short-term and do not provide evidence for long-term weight loss success. Taubes also argues that obesity is largely a hormonal disorder caused by insulin resistance, while Guyenet contends that obesity is a complex and multifactorial condition with a variety of genetic and environmental contributors.
Overall, Norton notes that the debate between Taubes and Guyenet reflects a larger debate in the nutrition and obesity research community about the relative importance of various factors in weight regulation. While the carbohydrate-insulin model has gained popularity in recent years, Norton argues that a more nuanced approach that considers the many factors that contribute to obesity is necessary for a comprehensive understanding of the condition, but he leans toward the CICO model, as the following bullet points and illustration of his depicts:
Dr. Layne Norton’s CICO Model
- Fat Balance = Fat Stored – Fat Burned
- If Stored > Burned then you are in a net positive fat balance and are gaining body fat
- If Burned > Stored then you are in a net negative fat balance and are losing body fat
- If Stored = Burned then you are in net fat balance and are maintaining body fat
Norton’s illustration below shows a representation of three meals, one set of low calorie/high fat (LCHF) and the other high calorie/low fat (HCLF).
At each meal, the LCHF diet is burning far more fat, but is also storing more fat. The HCLF group is burning much less fat but also storing much less fat. The overall net balance for each group is -50g fat per meal, or a -150g fat balance for three meals. This assumes that calories are equal between the two diets and that they are both in a negative energy balance (using more energy than ingesting).
The takeaway is that you can dramatically increase fat burning by eating a high fat diet, but burning more fat isn’t the same thing as losing more body fat because it only accounts for one side of the fat balance equation. When both parts of the story are accounted for we can see why carbs vs. fats don’t really make a difference on overall body fat loss, says Norton.
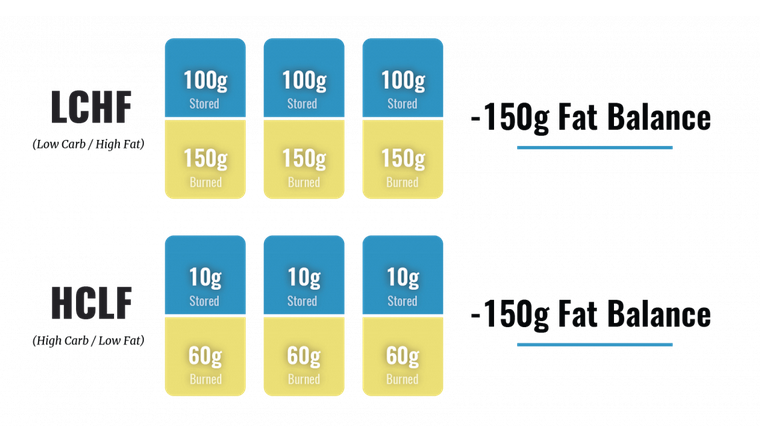
Fat balance as a function of fat stored minus fat burned (oxidized). The difference between stored and burned fat equals the net fat balance. In this example, a higher fat diet causes greater fat burning, but also greater fat storage compared to a calorie equated low fat diet that produces a lower rate of fat burning but also lower fat storage. The net fat balance between the two diets is equal.
In conclusion, CICO and CI both have scientific support, but caloric intake remains the most important factor for weight loss.
What about Keto?
Glad you asked.
The Problems with Keto
I think it’s important to discuss the Keto Diet because of its popularity. According to data from the International Food Information Council, 23 million Americans chose to follow a ketogenic, or “keto”, diet in 2021. If it’s harmful, it could harm many people.
Before I weigh in on the problems with Keto and why the Keto Diet struts around leaking a lot of nutrition misinformation, let’s get on the same page about what it is. For this, I turn to an article written by Ya’el Courtney, Keto — It’s Probably Not Right By You.
Ya’el Courtney is a PhD student at Harvard studying Neuroscience. She explains that the Keto Diet is a high-fat, low-carbohydrate diet that forces the body to burn fat for fuel instead of glucose (the CI model). She then delves into the potential negative effects of this diet on the body.
What Is the Keto Diet
Like I said, it’s a high-fat, low carb diet that is designed to make the body preferentially burn fat for fuel, rather than carbs.
The Keto Diet typically reduces total carbohydrate intake to less than 50 grams a day, with some people adhering to less than 20 grams a day. For context, one six-inch banana has 30 grams of carbohydrates, and one cup of cooked pasta has 45 grams. Keto dieters are encouraged to break down their daily caloric intake into approximately 70-80% fat, 10-20% protein, and 5-10% carbohydrates.
As Courtney reports, the brain requires a steady supply of about 120 grams of glucose each day. It cannot store glucose. This means that when carbohydrate intake is minimal or during fasting, the body goes hunting for some, and it’s found in the liver, which stores glucose as glycogen. After three to four days, the glycogen gets depleted and the body enters a state called ketosis. During ketosis, the liver becomes able to produce ketone bodies, a type of fuel made from stored fat. In theory, the body will then eat away at its stored fat to meet its energy demands, leading to fat loss in an individual.
Is Keto Good for Fat Loss
Here we go again with the CICO vs CI models.
If the CI model is accurate, then the high-fat/low-carb Keto Diet should promote greater weight loss than CICO.
Does it?
Well, as Courntey describes it, Keto should in theory burn fat, but in practice it may not. You can chalk this up to nutrition misinformation, because even though Keto dieters can experience initial weight loss, this is a short-term result from the loss of body water that accompanies lower carbohydrate intake, not fat loss.
This water loss happens because when carb intake exceeds energy they’re stored as glycogen molecules, and each gram of glycogen is stored with three grams of water attached to it. Thus, when you cut down on carbs, you quickly use up your glycogen stores, losing the associated water weight.
But there’s another issue that impacts weight loss on the Keto Diet — its restrictive design makes adherence unlikely; over 50% of people failing to adhere to a ketogenic diet in many medical studies, which negates any short-term weight loss effects.
Even if properly followed, a ketogenic diet is not intended to be adhered to long-term, nor is it uniquely effective, says Courtny. Studies show that after six months, a ketogenic diet does not lead to significantly higher weight loss than other weight loss approaches.
This conclusion was underscored by a 2016 study entitled Energy expenditure and body composition changes after an isocaloric ketogenic diet in overweight and obese men investigated the impact of an isocaloric ketogenic diet on energy expenditure, body composition, and various metabolic factors in overweight and obese men. The study involved 20 participants with an average body mass index (BMI) of 35 kg/m2, who consumed either an isocaloric (equivalent calories) ketogenic or a non-ketogenic diet for four weeks, while keeping their protein intake and total calorie intake constant.
The results of the study showed that the isocaloric ketogenic diet did not lead to a significant difference in energy expenditure or fat loss compared to the non-ketogenic diet, despite the significant difference in macronutrient composition. Both diets led to similar reductions in body weight, fat mass, and lean mass. The study also found no significant differences in fasting insulin, glucose, or lipid levels between the two diets.
More Problems with Keto Diet Misinformation
This high fat, moderate protein, low carbohydrate eating pattern is contrary to general healthful eating recommendations. It can lead to micronutrient deficiencies. Since the diet restricts many fruits, vegetables, and whole grains that are rich in vitamins and minerals, people following this diet may not get all of the necessary nutrients they need to maintain good health. Accordingly, people on the ketogenic diet have a higher risk of developing non-alcoholic fatty liver disease, which can lead to liver damage and other health problems.
Another potential drawback of the ketogenic diet is that it can be difficult to stick to long-term. The diet can be very restrictive, and people may find it challenging to maintain the high-fat, low-carb eating pattern over an extended period of time. Additionally, the article mentions that the diet may lead to bad breath, constipation, and other uncomfortable side effects.
There’s also a food quality issue. The focus of the diet is on macronutrient ratios, rather than the quality of the food being consumed. This can lead to people on the diet eating unhealthy processed foods, such as bacon and cheese, instead of nutrient-dense whole foods.
The researchers concluded that an isocaloric ketogenic diet is not superior to a non-ketogenic diet in terms of energy expenditure and body composition changes in overweight and obese men when protein and calorie intake are held constant.
What is better than Keto?
The Mediterranean Diet!
Go Mediterranean!
U.S. News & World Report ranked the Mediterranean diet No. 1 on its 40 Best Diets Overall list for 2022, citing a “host of health benefits, including weight loss, heart and brain health, cancer prevention, and diabetes prevention and control.”
UPDATE 5/14/23: A day after I published this post, the estimable Dr. Brad Stanfield put out a video reviewing three studies published this year that independently confirmed the best diet for human health.
Here’s the video, and below it a summary of it:
The studies reviewed in the video above analyzed different diets: low carbohydrate, low-fat, ketogenic diet and the Mediterranean Diet. Thanks to Prabhjeet Singh for the following summary.
The first study, published in the Journal of Medicine, was a prospective cohort study comparing low carbohydrate diets to low-fat diets. It was a massive observational study involving over 371,000 participants between the ages of 50 to 71 years old in the United States. The study found that those following a low carbohydrate diet had increased rates of death, heart disease, and cancer. The study indicated that a healthy low-fat diet with minimal saturated fat intake would be an effective dietary strategy for healthy aging.
The second study, published in the British Medical Journal, was a systematic review and meta-analysis. It found that the Mediterranean Diet and low-fat diets were most effective in reducing all-cause death rates.
The third study was a narrative review discussing the Mediterranean Diet and its benefits in limiting many culprits in the standard American diet (SAD) that drive cardiovascular disease. It also discussed the Keto and other very low carbohydrate diets, stating that while they have been promoted for effects on weight loss, improvement in insulin resistance, and blood sugar level control, they can also promote increases in LDL cholesterol.
The bottom line:
All three studies suggest reducing low quality carbohydrates and saturated fats and replacing those with high-quality proteins.
What Is the Med Diet and What Is It Good For?
The Mediterranean Diet is a highly-regarded eating pattern that emphasizes plant-based foods and healthy fats. It’s characterized by an abundance of vegetables, fruits, whole grains, beans, lentils, nuts and extra virgin olive oil. Moderate amounts of fish, cheese, yogurt, and poultry are also included, while red meat, butter, sweets, and sugary drinks are limited.
My post, The Blue Zone Diet Will Transform You, shows that different ethnicities living in distinct places around the world (the “Blue Zones”) that adhere to this diet, the Med Diet, live longer and healthier than anywhere else in the world.
According to a robust study, this diet may help prevent heart disease, stroke, and certain types of cancer. Another study found that adherence to the Mediterranean Diet is associated with a lower risk of mental health issues. Furthermore, a third study showed that this eating pattern can lower the risk of chronic diseases such as type 2 diabetes.
By limiting unhealthy fats, sodium, and refined carbohydrates, while promoting healthy unsaturated fats, fiber, and antioxidants, the Med Diet can promote healthy blood sugar, blood pressure, cholesterol, and gut microbiota, leading to a longer lifespan and reduced risk of chronic diseases.
EveryDayHealth.com summarized studies that showed the Med Diet can help:
- Reduce heart disease risk
- Reduce risk of stroke in women
- Prevent cognitive decline and Alzheimer’s
- Help with weight loss and maintenance
- Stave off type 2 diabetes
- Relieve rheumatoid arthritis symptoms
- Help protect against certain kinds of cancers
- Ease depression
(Go here to read about any on the above list)
Mediterranean Diet’s Cellular Effects Revealed
People who follow the Mediterranean diet—rich in fats from olive oil and nuts—tend to live longer, healthier lives than others who chow down primarily on fast food, meat and dairy. But it hasn’t been clear on a cellular level exactly why the diet is so beneficial.
Science is getting closer to finding out, beginning in the case I’m about to tell you about, with worms.
I know you’re not a worm, but a some of their biology is similar to ours, such as the mechanisms behind lipotoxicity. (Deleterious effects of lipid accumulation in non-adipose tissues are known as lipotoxicity.)
So, some features of the Med Diet were tested on worms in a study entitled Lipid droplets and peroxisomes are co-regulated to drive lifespan extension in response to mono-unsaturated fatty acids. The researchers investigated the molecular mechanisms that contribute to lifespan extension in response to mono-unsaturated fatty acids (MUFAs). They found that MUFAs, such as oleic acid found in olive oil, induce the formation of lipid droplets and the activation of peroxisomes, leading to lifespan extension in worms.
The study provides important insights into the underlying mechanisms that drive the well-known health benefits of the Mediterranean diet, which is rich in MUFAs. MUFAs stimulate the formation of lipid droplets, which act as reservoirs for fatty acids and help protect cells from lipotoxicity. The lipid droplets also promote the formation of peroxisomes, which are organelles that are involved in fatty acid metabolism and detoxification.
The researchers learned that one of the fats in the Mediterranean diet, oleic acid, increases the number of two key cellular structures, or organelles, and protects cellular membranes from damage by a chemical reaction called oxidation. This protective effect has a big payoff: Worms fed food rich in oleic acid lived about 35% longer than those consigned to standard worm rations, the researchers found.
The study’s findings suggest that the co-regulation of lipid droplets and peroxisomes may play a key role in promoting health and longevity, and could potentially be targeted to develop interventions to prevent age-related diseases. In particular, the study’s authors suggest that the stimulation of peroxisome formation may be a promising target for therapeutic interventions aimed at promoting healthy aging.
Start Eating Mediterranean
You can read about how to cook Med meals, or watch them getting made.
Readers:
Read these 30 Mediterranean meal recipes
Watchers:
Mediterranean Diet for Beginners – YouTube
Mediterranean Diet | Quick, Easy and Flexible Healthy Recipes
Take the plunge. The Med is warm and inviting.
Last Updated on February 7, 2024 by Joe Garma








