Why Intermittent Energy Restriction and Circadian Rhythms Optimize Your Health
Intermittent Energy Restriction has been tested now with both animals and people. So has the effects of circadian rhythms. The results are clear — if you consistently under-eat on certain days and end your “feeding window” soon after dark, your will live healthier longer and resist age-related chronic diseases.
WE GROW up being told that we need to eat three meals a day, that you shouldn’t skip breakfast, and metabolism is enhanced by eating several small meals throughout the day.
I don’t want to entirely disabuse you of these notions, because in certain situations any of those bromides may be relevant to you. For instance, if you skip a meal and then wind up consuming even more calories later in the day, it makes sense to eat at regular, consistent intervals so that you’re not to hungry before any one meal.
If you workout two or more times a day, or have an issue with hypoglycemia, then eating every two or three hours may be useful.
If, however, you want to maximize your healthspan, perhaps even your lifespan, then you might consider two things:
- Practice some regimen of fasting and/or caloric restriction; and
- Narrow your “feeding window” such that it’s harmonious with your circadian clock, and that in effect means, don’t eat at night.
Even if you’d rather choke on ice cream cake at midnight, rather than consider tempering when you eat, or not eat at all — do yourself a favor and at least skim this piece for a few nuggets that just may improve your life.
In this article, we’ll cover:
- Why ubiquitous food and artificial light make us sick and fat;
- How timing your meals to your circadian clock improves health;
- Why Intermittent Energy Restriction and fasting improve your vitally important cellular and molecular mechanisms involved in removing metabolic waste and reducing systemic inflammation; and
- A quick summary of of it all in “Your Takeaway”.
What follows is a summary a scientific report entitled, Meal frequency and timing in health and disease. Yes, I could have simply provided an introduction to the study and said, “Have at it”, but then all but the most patient and scientifically-inclined of you would have taken one look, gasped, and then clicked away.
I nearly did myself. But insanity took over and I waded in, looked up terms, reorganized things, added some phrases most people can understand… and about 15 hours later, here we are.
Note: All the assertions herein made are footnoted in the original study, so go there if you’d like to dig deeper. And, of course, there’s always Google.
Now, let’s dig in…
Why Ubiquitous Food and Artificial Light Make Us Sick and Fat
The agricultural revolution has cut both ways, good and bad.
On the one hand, it created food security in that food could be regularly grown, harvested and stored, thus alleviating the need to constantly hunt and gather food, and be vulnerable when it wasn’t accessible.
On the other hand, the downside of the agricultural revolution is that alleviated the need for most of us to expend energy to obtain food and provided the capability to adopt a three meals per day eating pattern.
Moreover, during the last 50 years, food has become increasingly processed, much of it now made to be calorically dense with refined grains, sugar, cooking oils, corn syrup, preservatives, etc.
When a population with a sedentary lifestyle regularly consumes high-energy meals multiple times each day, it experiences obesity and related metabolic diseases (like diabetes) that are the major causes of morbidity and mortality in our world today. Hunter-gatherer humans rarely, if ever, suffer from obesity, diabetes, and cardiovascular disease.
The rising tide of obesity is strongly associated with daily calorie intake and sedentary lifestyle-promoting transportation
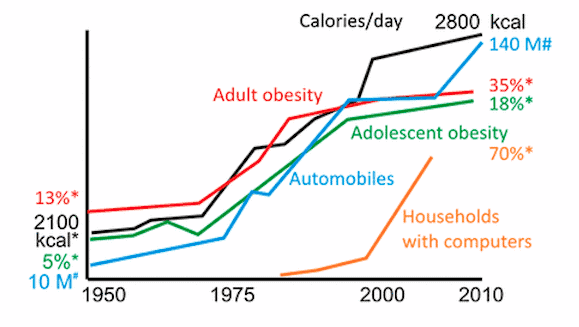
*US, approximate value. #Worldwide auto production. (Credit: http://www.pnas.org/content/111/47/16647.long#xref-ref-19-1)
Take a look at the above graph and note how the growth of obesity (red and green) correlates with the growth of two things that keep your butt in seat. I refer to automobiles and computers, during which time caloric intake moved up from 2,100 to 2,800 per day.
It’s been a double whammy — on one hand more calories from ever-present food, and on the other hand less need to move our bodies. Neither fits how we evolved.
From an evolutionary perspective, the most common eating pattern in modern societies — three meals plus snacks every day — is abnormal.
Emerging findings from studies of animal models and human subjects suggest that Intermittent Energy Restriction periods of as little as 16 hours can improve health indicators and counteract disease processes. (So, for instance, you eat during an eight hour window, say 1:00 PM — 8:00 PM, and fast for 16 hours, starting at 8:00 PM and lasting through the sleep cycle and next morning till 1:00 PM.)
The relevant mechanisms that improve health/counteract disease involve a metabolic shift to fat metabolism and ketone production, and stimulation of adaptive cellular stress responses that prevent and repair molecular damage.
Although I’m mostly going to focus on Intermittent Energy Restriction, another two experimental dietary regimens will be covered. In toto, they are:
- Caloric Restriction (“CR”), in which daily calorie intake is reduced by 20–40%, and meal frequency is unchanged;
- Intermittent Energy Restriction (“IER”), which involves eliminating (fasting) or greatly reducing (e.g., 500 calories per day) the daily intake of food/caloric beverage intermittently, for example 2 days per week; and
- Time-restricted Feeding (“TRF”), which involves limiting daily intake of food and caloric beverages to a 4 to 6 hour time window. (TRF schemes can be up to 12 hours, but time frames over 6 hours were not used in produce the outcomes herein described.)
By the time you finished reading this, hopefully you’ll want to experiment with one or more.
How Timing Your Meals To Your Circadian Clock Improves Health
Yes, its true, says the science — improve your healthspan and become resistant to disease by letting your circadian rhythms guide your feeding window.
Your circadian clock strongly influences your behavior, physiology, and metabolism
Sometimes it’s called a “circadian clock”, sometimes “circadian rhythms”, or your “sleep/wake cycle”, but irrespective of the term, you know what this is, because you experience it regularly.
If you’ve ever noticed that you tend to feel energized and drowsy around the same times every day, you have your circadian rhythm to thank or disparage.
What is it, exactly?
Your circadian rhythm is basically a 24-hour internal clock that is running in the background of your brain and cycles between sleepiness and alertness at regular intervals. This “clock” governs self-sustained 24-hour oscillations in behavior, physiology, and metabolism.
Gene-expression studies have revealed more than 10% of expressed genes in any given organ exhibit circadian oscillation, which regulates and optimizes your fitness beginning on the cellular level. This is accomplished by a tiny part of the brain called the SCN (hypothalamic suprachiasmatic nucleus) within the hypothalamus.
The above image illustrates the photoreceptive retinal ganglion cells in your eye’s retina sending ambient light information to the SCN to ensure that the circadian system is entrained to the daily light/dark cycle, profoundly affecting both your physiology and behavior.
Our use of artificial light, work and eating habits can disrupt our “clock” and our health
All diurnal animals, like us, are tuned to light. For millions of years of our existence prior to artificial light, the circadian clock—in conjunction with the retinal light input—imposed diurnal rhythms in physiology and behavior, including the activity/rest and feeding/fasting cycle.
For most of human existence food was often scarce and primarily consumed during daylight hours, leaving long hours of overnight fasting. Then affordable artificial light was disseminated to much of the world’s population, and we modern humans experienced prolonged hours of illumination, which afforded us extra hours of eating.
Think about it — it’s nighttime, most of us no longer need to ingest calories for energy since we’re no longer active, but we flip on the light switch and keep eating.
Our modern lifestyle upset our circadian system in three primary ways:
- Shift work,
- Exposure to prolonged hours of artificial light, and
- Erratic eating patterns.
Let’s look at how these impact the mechanisms and consequences of circadian disruptions.
Shift work can create chronic circadian disruptions resulting in disease
Nearly 10% of the workforce in industrial societies performs night-shift work whereby the individuals are subject to both prolonged hours of artificial lighting and an abnormal eating schedule. Then during the weekend, the tendency is to maintain a day-active social life, which imposes a jet-lag–type paradigm where both central and peripheral clocks attempt to adjust to a weekend lifestyle.
Researchers have yet to get definitive proof from human studies, but based on animal experimental work shift work is presumed to result in chronic disruption of circadian rhythms, which may help explain the known association between night work and several diseases, including cardiovascular disease, diabetes, obesity, certain types of cancer, and neurodegenerative diseases.
When you eat is more important than what you eat (Read this too.)
We now know that prolonged illumination and erratic eating patterns disrupt the circadian system.
Consider these findings:
- In nocturnal rodent studies, extended illumination has been shown to increase predisposition to metabolic diseases. Conversely, in diurnal flies a shift to nighttime feeding compromises fat metabolism and fecundity.
- In other words, when either rodents or flies ate past what their circadian clocks dictated, bad things happened.
- In humans a 12 hour shift of the sleep/wake and fasting/feeding cycle while maintaining a moderate-carbohydrate, moderate-fat diet that allows them to eat whatever they want as long as they consume the same amount of carbohydrates, proteins and fats daily (an “isocaloric diet”), resulting in reduced glucose tolerance, increased blood pressure, and decreased the satiety hormone leptin.
- In other words, when people have a consistent diet consumed only during a 12 hour feeding window, good things happen.
- Expanding on the point immediately above, Time Restriction Feeding (“TRF”) is effective even when not altering caloric intake or source of calories, suggesting that reducing the hours within which you eat and minimizing the time you eat at night will garner metabolic benefits and is a good weight-loss therapy, particularly in overweight an obese people.
Improve Your Vitally Important Cellular and Molecular Mechanisms With Intermittent Energy Restriction and Fasting
It’s been clearly shown in studies of various organisms from yeast and worms, to mice and monkeys, that those with dietary energy (caloric) restrictions experience extended healthy lifespans as compared to those who ate whatever and whenever they wanted (fed “ad libitum”).
Intermittent Energy Restriction (“IER”) can forestall and even reverse disease processes in animal models of various cancers, cardiovascular disease, diabetes, and neurodegenerative disorders.
Obviously, lifespans of humans are harder to study than shorter-lived organisms; however, data collected from individuals practicing severe dietary restriction indicate that humans undergo many of the same molecular, metabolic, and physiologic adaptations typical of long-lived Calorie Restricted (“CR”) rodents.
Let’s take a look at four mechanisms by which IER protects cells against injury and disease.
1. Adaptive Stress Responses Improve With Intermittent Energy Restriction
The most conclusive results from IER studies come from animal tests, but the scientists who conduct them believe that humans are likely to experience similarly impaired health if they eat ad libitum, and similarly robust healthspans if they maintain IER.
Animals on IER obtain a heightened adaptive stress responses at the molecular, cellular, and organ system levels, which include:
- Prevent of age-related declines in the antioxidant enzyme superoxide dismutase 1 that breaks down a type of free radical called superoxide.
- Increase levels of the antioxidant enzymes NADH-cytochrome b5 reductase and NAD(P)H-quinone oxidoreductase 1 in muscle cells of mice, the beneficial effects of which were accentuated by exercise.
- Protect neurons against oxidative, metabolic, and proteotoxic stress in animal models of neurodegenerative disorders, including Alzheimer’s and Parkinson’s diseases.
- Promote neuronal survival, neurogenesis and the formation and strengthening of synapses in the brain.
- Stimulate the production of several different neuroprotective proteins (essential proteins for brain function with a role in normal cognitive performance), including the antioxidant enzyme heme oxygenase 1, proteins involved in mitochondrial function, and the protein chaperones HSP-70 and GRP-78.
The net of all those bullet points packed with technical jargon is that the beneficial effects of IER involve the general biological phenomenon of “hormesis” or “preconditioning,” in which exposure of cells and organisms to a mild stress results in adaptive responses that protect against more severe stress.
So, yes an IER regimen does produce a small amount of stress because you’re under-eating; however the body adapts to that by becoming stronger and more resilient, giving credence to German philosopher,
Friedrich Nietzsche, who said:
That which does not kill us, makes us stronger.
2. The Bioenergetics of Cellular, Metabolic and Enzymatic Processes is Improved with IER
There are several ways to do an Intermittent Energy Restriction diet.
Remember, with IER the point is to eliminate or substantially reduce your daily caloric intake over a certain period of time.
Three well-studied Intermittent Energy Restriction configurations are:
- 5:2 Diet, made popular by the BBC’s Dr. Michael Mosley’s book, The Fast Diet. With 5:2, you eat your normal diet for five days a week and then eat an Energy Restricted (“ER”) diet on the two remaining days. The number of calories ingested during the ER days varies, often depending on your size, energy expenditure and/or fortitude. The range of calories ingested typically used in studies is between 500 and 600 per day during the ER days.
- Alternate Day ER, whereby you limit calories per the ER part of the 5:2 diet described above on one day, and eat normally the next; repeat.
- Alternate Day Fast, whereby you eat normally on one day and do a water-only fast the next day; repeat.
If you already haven’t realized it, I want to underscore that it’s truly worth experimenting with IER.
When humans switch from eating three full meals per day to an IER diet, such as one moderate size meal every other day or only 500–600 calories for two days per week, they exhibit robust changes in energy metabolism characterized by increased insulin sensitivity, reduced levels of insulin and leptin, mobilization of fatty acids, and elevation of ketone levels.
(Ketones, such as β-hydroxybutyrate (found in butter), are known to have beneficial effects on cells with a high energy demand, such as neurons in the brain. Is the Ketone Diet for you?)
Consider these multiple benefits to blood sugar moderation (insulin sensitivity), energy, brain function and cancer-resistance:
- In humans IER can increase insulin sensitivity more than daily calorie restriction that achieves similar weight loss.
- The benefit here is that studies show people can sustain IER better than daily caloric deprivation.
- Dietary energy restriction can prevent age-related decline in mitochondrial oxidative capacity in skeletal muscle, and can induce mitochondrial biogenesis.
- This means that you won’t get as tired and energy-zapped as you age if on IER.
- Brain bioenergetics may also be bolstered by IER. For example, brain-derived neurotrophic factor (BDNF), which is up-regulated in hippocampal neurons in response to IER and exercise, activates the transcription factor CREB, which then induces peroxisome proliferator-activated receptor gamma coactivator 1-α (PGC-1α) expression and mitochondrial biogenesis.
- That big mouthful of science words means that IER can make your brain work better, longer.
- Animal models consistently show that IER inhibits and even reverses the growth of a range of tumors, including neuroblastoma, breast, and ovarian cancers. The shift to ketogenesis may play an important role in suppression of tumor growth by IER/fasting because many tumor cells are largely unable to use ketones as an energy source; accordingly, ketogenic diets may potentiate the anti-tumor effects of IER.
- This is one research focus of Dr. Valter Longo. He’s convinced that cancer outcomes can be improved by eliminating sugar and carbohydrates (other than vegetables, mostly) from the diet.
- Although the animal models have been more extensively studied, recent case studies in human patients suggest potential applications of IER in the treatment of a range of cancers, including breast, ovarian, prostate, and glioblastoma.
- Interestingly, evolutionary theory predicts that collected random mutations will prevent tumor cells from making the necessary metabolic adaptations to IER.
3. IER Reduces Systemic Inflammation, Associated with Many Chronic, Age-related Diseases
All major diseases involve chronic inflammation in the affected tissues and, often, systemically. This includes cardiovascular disease, diabetes, neurodegenerative disorders, arthritis, and cancers.
Let’s take a peek on Intermittent Energy Restriction’s affects on a few chronic health issues.
Overweight and Obesity: IER suppresses the inflammation associated with overweight and obesity in both human subjects and animal models. Obese women who changed their diet from multiple daily meals to alternate-day energy restriction exhibited significant reductions in levels of pro-inflammatory proteins that are involved in systemic inflammation; namely, circulating TNF and IL-6.
Asthma: Two months of alternate-day energy restriction reduced circulating TNF and markers of oxidative stress, and also improved asthma symptoms and airway resistance. That said, because weight loss may reduce inflammation irrespective of the dietary change inducing the weight loss, more research is needed to determine if and how eating patterns modify inflammation independent of weight loss.
Rheumatoid Arthritis, MS, Lupus, Type 1 Diabetes: Multiple studies have shown that fasting can lessen symptoms in patients with rheumatoid arthritis. Data from animal studies suggest that the pathogenesis of other autoimmune disorders may also be counteracted by IER, including multiple sclerosis, lupus erythematosus, and type I diabetes.
Stroke: In a mouse model of stroke, IER suppressed elevations of the pro-inflammatory proteins TNF and IL-1β in the ischemic cerebral cortex and striatum, which was associated with improved functional outcome.
Cancer: Inflammation is increasingly recognized as a contributing factor for cancer cell growth. Given that excessive energy intake (e.g excessive calories) promotes inflammation, it’s likely that suppression of inflammation plays a role in the inhibition of tumor growth by IER.
4. IER Improves Repair and Removal of Damaged Molecules and Organelles
Cells possess dedicated mechanisms for the removal of damaged molecules and organelles, but these processes are hampered by energy (caloric) intake, especially if excessive (over eating).
Two mechanisms designed to “cleanse” the body of unwanted molecules, organelles and other “debris”, involves ubiquitin and autophagy. (Here’s what you need to know about autophagy.)
Ubiquitin is a regulatory protein found in most tissues. The process of “ubiquitination” damaged proteins are “tagged” with ubiquitin, making them targets for degradation.
In the second mechanism, autophagy, damaged and dysfunctional proteins, membranes, and organelles are directed to and degraded in lysosomes, which are membrane-bound organelles found in nearly all animal cells and havehydrolyticenzymes that can break down virtually all kinds of biomolecules.
The important thing to focus on here is that energy and nutrient intake (particularly amino acids) have been shown to have consistent effects on autophagy. When organisms ingest regular meals, their cells receive a relatively steady supply of nutrients and so remain in a “growth mode” in which protein synthesis is robust and autophagy is suppressed. The nutrient-responsive mTOR pathway negatively regulates autophagy.
We don’t want autophagy to be suppressed (“negatively regulated”); instead, we want this mechanism to “clean up” any cellular debris, etc. that if left to accumulate, contributes to disease.
One good way to encourage autophagy is to fast, either completely on a regular basis, or via some form of Intermittent Energy Restriction. Fasting inhibits the mTOR pathway and stimulates autophagy in cells of many tissues, including liver, kidney, and skeletal muscle. In this way, fasting “cleanses” cells of damaged molecules and organelles.
In addition to the frequency of meals, the circadian timing of meals is likely to affect the responses of the cellular machinery for clearance of damaged proteins and organelles. Autophagy is regulated in a diurnal rhythm in many cell types, and this rhythm can be altered by changing the timing of food intake. It is therefore reasonable to consider that meal timing has an impact on diseases that involve impaired or insufficient autophagy.
Your Takeaway
Yes, this blog post is long and complicated, so let me deconstruct it a bit.
Remember these three things:
- Humans evolved to eat and then fast, simply because food was not always available.
- Fasting, which includes under-eating, enables the repair and removal of damaged molecules and organelle — a clean-up process that improves cellular health, as well as reducing systemic inflammation, a precursor/promoter of most chronic diseases.
- Our circadian clock governs the effectiveness of various metabolic functions and pretty much insists that we stop eating at night (just like in the good old days prior to artificial light) if we’re to stay healthy and resistant to age-related chronic diseases.
Try one or more of these three things:
- Choose two days back-to-back when you under-eat. If you’re worried that you’ll starve, try reducing calories by just 30% and incrementally keep reducing till you’re ingesting 500 to 600 calories on those under-eat days.
- Alternate between normal eating and under-eating. Day 1 normal, day 2 under-eat, etc. Like above, as you get the hang of it, reduce the amount of calories on the under-eat days.
- Try what I do, which is a mode of intermittent fasting whereby I begin eating at 1:00 PM and stop by 8:00 PM. Over time I hope to bring the quit-eating-time down to 7:00 PM, which is more aligned with our circadian clock. A caveat: If you exercise regularly and with some intensity, over-eat on one of those days to replenish your carbohydrate stores.
Finally, if you do any of this, adopt the proper mindset, which is a light-hearted experimental attitude infused by the corresponding actions and participation of a buddy or two. This mindset will hopefully keep you from being too self-critical, and your buddies will help you stay on the path (compliance) and have fun.
Get to it!
P.S Don’t miss reading, When You Eat Is More Important Than What You Eat, Says Dr. Panda.
Last Updated on February 7, 2024 by Joe Garma








