Why The Right Gut Bacteria Is Essential To Good Health and How Antibiotics Kills It All
The right foods and supplements will nourish the right gut bacteria so necessary for overall health and longevity. Learn why gut health is the key to your vitality, and why antibiotic drugs kills it all.
IT WAS the third call I got from her this week, and there was fear in her voice:
“You know, that infection I told you about… well, I went to my doctor again and he prescribed a really strong antibiotic with some scary side effects. I don’t want to do this!”
Thankfully, my friend, Dara, didn’t have to. She took a natural alternative and within two days her symptoms had eased considerably. Moreover, she didn’t kill off the beneficial bacteria in her gut, which, unfortunately, antibiotics do very effectively; they don’t discriminate between the good and the bad.
I’ll tell you about the infection she had and what natural remedy she took to beat it into submission, but first I want to tell you why it’s so important to avoid antibiotics and maintain your gut health.
The first reason is that too many people are taking too many antibiotics too often, which then exposes them to too many bacteria and too many antibiotics, resulting in the evolution of superbugs.
Bacteria become superbugs because they are adept at developing immunity to antibiotic drugs. Currently, there’s a world wide superbug crisis because such bacteria are becoming resistant to antibiotics.
The second reason that you should do all you can to avoid taking antibiotics is that they kill the beneficial bacteria in your gut.
Why should you care about that?
Simply because the beneficial bacteria in your gut are called “beneficial” for a reason; to wit, they strongly influence your body fat, inflammation level, propensity for metabolic syndrome, your immune system, brain health and more.
And it’s not just antibiotics kill off these beneficial buggies — as you’ll soon see, sugary, processed foods and drinks have a similar effect by changing the important ratio between beneficial and harmful bacteria, thereby potentially making you fatter, more prone to chronic disease and cognitively challenged.
As Dr. Mark Hyman puts it:
If you want to fix your health, start with your gut. Gut health literally affects your entire body.
In this article, you’ll discover:
- Why antibiotic drugs are dangerous.
- Why weight loss requires the right gut bacteria.
- How the right gut bacteria can reduce inflammation and metabolic syndrome.
- That you need the right gut bacteria for brain health, including cognitive capacity and mood.
- Why you need the right Firmicutes to Bacteroidetes ratio.
- How to properly feed your beneficial gut bacteria.
- What are the best prebiotic and probiotic supplements.
- 5 natural antibiotics that are good for your beneficial gut bacteria, and thereby, good for you.
Let’s dig in…
You Need the Right Gut Bacteria for Weight Loss
In an article about gut the bacteria beneficial for weight loss, dietitian Lea Basch explains how the right kind of bacteria can help you become (or remain) lean, and the wrong kind can contribute to weight gain.
Dr. Raphael Kellman, author of The Microbiome Diet, puts it this way:
“Simply put, if you get the microbiome—that collection of bacteria inside you—healthy, you will lose weight. It’s less about eating a certain percentage of carbohydrates, protein, and fat than about correcting the overgrowth of unhealthy bacteria, which is making you crave the wrong foods, triggering inflammation.”
Lea Basch lists three reasons improving your balance of good bacteria to bad bacteria may aid in weight loss:
(1) Different bacteria in your gut extract different amounts of nutrients. For instance, the Firmicutes bacterial strain converts food to calories at a greater rate than Bacteroidetes; therefore, to lose weight it’s helpful to increase Bacteroidetes and decrease Firmicutes.
(2) A healthy gut helps produce dopamine and serotonin. These two feel-good neurotransmitters are produced in the gut and affect the brain by suppressing moodiness, depression and anxiety, thereby decreases stress-related eating.
(3) Some unhealthy gut bacteria can increase chronic inflammation, which in turn can increase appetite and insulin resistance, causing unhealthy food cravings and suppressing the immune system.
For more about how gut bacteria affects body weight, and what a study of twins reveals (one fat, one thin), read my article, Get The Right Gut Bacteria For Weight Loss.
Conclusion:
You Need The Right Gut Bacteria To Reduce Inflammation
Let’s further explore that notion of how bacteria affects inflammation, beginning with Dr. Paresh Dandona, a diabetes specialist in Buffalo, New York, who wanted to know what happens within minutes of eating a McDonald’s breakfast of an egg sandwich with cheese and ham, a sausage muffin sandwich, and two hash brown patties.
As scientist-types do, Dr. Dandona conducted an experiment to find out. The results were startling!
Over several mornings, he fed nine normal-weight volunteers that aforementioned McDonald’s breakfast, one regularly eaten by a large swath of Americans, as well as many others worldwide. He was shocked to find that levels of a C-reactive protein — an indicator of systemic inflammation — dramatically surged within minutes.
And the inflammation lasted for hours.
Why be concerned with inflammation, you ask?
Well, chronic inflammation either helps promote and/or magnifies the deleterious affects in various “wear and tear” conditions, including osteoarthritis, and autoimmune diseases, such as lupus and rheumatoid arthritis, allergies, asthma, inflammatory bowel disease and Crohn’s disease.
But, as they say, there’s more!
As Live Science reports, chronic inflammation is also involved in heart disease, diabetes, lung issues, bone health and depression. Because it’s such a big part of so many chronic illnesses that gradually become more debilitating as we age, there’s now a new term for it, inflammaging.
As this PubMed abstract puts it:
“Human aging is characterized by a chronic, low-grade inflammation, and this phenomenon has been termed as “inflammaging.” Inflammaging is a highly significant risk factor for both morbidity [a diseased state] and mortality [death] in the elderly people, as most if not all age-related diseases share an inflammatory pathogenesis [how the disease develops].”
A 2015 study in JAMA Psychiatry found that people with depression had 30% more brain inflammation than those who were not depressed. Furthermore, inflammation has been linked to symptoms of depression, including feeling down, loss of appetite and sleep problems. Scientists remain unsure of why inflammation is linked to sleep problems or low moods, but suspect that cytokines can interfere with hunger signals.
Guess what, there’s even more!!
Back to Dr. Dandona. His focus was on if and how inflammation could contribute to causing Metabolic Syndrome, a term that refers to a group of risk factors that raises your chances of getting diabetes, heart disease, stroke, certain cancers, and even dementia—the top killers of the developed world.
Here’s a snapshot of what characterizes Metabolic Syndrome:
Dr. Dandona spent a decade testing the effects of various foods on the immune system in order to determine if chronic inflammation was a significant cause of metabolic syndrome. His breakthrough moment came when he discovered that certain foods with near identical characteristics could have a completely different effect on the body due to something quite small and oft neglected.
If you have three or more of the above listed biometrics of Metabolic Syndrome, read more about Dr. Dandona’s discoveries.
When you’re done with that, go to Part 2 where you can learn how a microbiologist named Dr. Liping Zhao, who had three of the five attributes for Metabolic Syndrome, lost 44 pounds, normalized his blood pressure and reduced his LDL (the “bad” cholesterol).
I’ll give you a heads up. Liping Zhao did two simple things:
- He changed his diet to whole grains, rich in those prebiotic fibers important for beneficial bacteria; and
- He began regularly consuming two traditional medicinal foods thought to have such properties: bitter melon and Chinese yam.
For more on what to do to help with Metabolic Syndrome, read my article, How Gut Bacteria Increase The Chance You’ll Suffer From Metabolic Syndrome And A Simple Solution.
Conclusion
You Need The Right Gut Bacteria For A Strong Immune System

Credit: https://www.npr.org/sections/goatsandsoda/2014/11/14/363375355/how-bacteria-in-the-gut-help-fight-off-viruses (Click pic to enlarge)
Your gut wall houses 70% of the cells that make up your immune system, says Dr. Hyman.
A study called, The role of gut microbiota in immune homeostasis and autoimmunity made these observations:
“The gut microbiota that resides in the gastrointestinal tract provides essential health benefits to its host, particularly by regulating immune homeostasis [stability, balance, or equilibrium of the immune system]. Moreover, it has recently become obvious that alterations of these gut microbial communities can cause immune dysregulation [immune system dysfunction], leading to autoimmune disorders.”
The study goes on to highlight:
- The importance of inflammation as a major cause of dysbiosis and disease. (Dysbiosis is an undesirable shift in the microbiota composition, resulting in an imbalance between protective and potentially harmful microbes that can damage the gut lining and lead to chronic diseases.)
- The right gut bacteria (called “beneficial” or “commensal” bacteria) to help improve various diseases, includes:
- B. fragilis
- Bacteroides thetaiotaomicron
- L. paracasei DSM 13434
- L. plantarum DSM 15312 and DSM 15313
There’s simply no way you can have a healthy immune system without the critically helpful participation of the right gut bacteria.
Conclusion
You Need the Right Gut Bacteria for Brain Health
A growing body of preclinical literature has demonstrated that the brain and gut are connected via multiple neuroendocrine signalling mechanisms.
(The neuroendocrine system is the mechanism by which the hypothalamus maintains homeostasis, regulating reproduction, metabolism, eating and drinking behavior, energy utilization, osmolarity and blood pressure.)
What this means is that changes to to the gut microbiome can affect emotional behavior and related brain systems, either for good or ill.
It’s now clear that alterations in the gut microbiome may play a disordered physiological process associated with disease or injury (“pathophysiological role”), including autism spectrum disorder, anxiety, depression, and chronic pain.
Back to Dr. Hyman. He makes the following points about our “gut-brain connection”:
- Our gut nervous system acts as a second brain. Researchers find the gut-brain connection plays an important part in gastrointestinal function, but also influences feelings and intuitive decision-making.
- Besides your brain, your gut is the only organ with its own nervous system. Your small intestine alone has as many neurons as your spinal cord. Your gut nerve cells produce 95 percent of serotonin, and every class of neurotransmitter in your brain also resides in your gut. Your gut, in fact, contains more neurotransmitters than your brain.
- Your gut must be completely in balance for your brain to be in balance. Gut-brain disturbances manifest in a wide range of disorders, including functional and inflammatory gastrointestinal disorders, obesity and eating disorders.
You should need no more convincing to focus on cultivating the right gut bacteria than the following graph:
Cognitive Decline with Age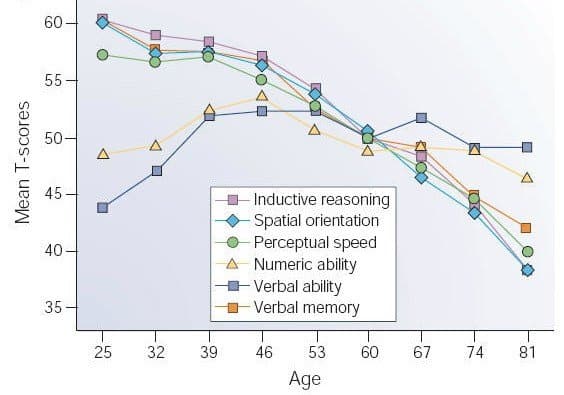
Every measure of cognition — inductive reasoning, spatial orientation, perceptual speed, numeric ability, verbal ability and verbal memory — declines as we age. Ensuring that your microbiome is populated with the right beneficial bacteria is a major factor to maintain cognitive health.
For more on the gut-brain connection, read my article, Get The Right Gut Bacteria for Brain Health, Part 2: The “Gut-Brain” Axis, where you can also get a list of specific Bifidobacterium and Lactobacillus strains that have beneficial effects on anxiety and depression-like behavior.
Conclusion
You Need the Right Gut Bacteria to Extend Your Lifespan
The right gut bacteria has been shown to extend the lifespan of mice, but the research also suggests that the right gut bacteria might assist we mere humans in extending our lifespan as well.
“A diet supplemented with a specific probiotic bacterial strain increases the lifespan of mice. The mammalian gut [that includes ours] is home to hundreds of bacterial species that contribute to food digestion and, in some cases, inflammatory gut diseases. Probiotics, beneficial bacterial species, can enhance gut health by keeping the resident bacteria in check.”
So, how much longer did those mice live, and what specific probiotic strain did the job?
In one sec I’ll tell you, but first know that the increased longevity happened because of what the probiotic strain did to relieve the mice of inflammation, which was previously shown to do the same — reduce inflammation — in elderly humans, although the lifespan part wasn’t tested.
What Was The Probiotic Strain that Increased Lifespan?
The probiotic bacterial strain Bifidobacterium animalis, subspecies lactis LKM512 did the trick, and as mentioned, this strain also reduced inflammation in humans.
How Much Longer Did The Mice Live?
The researchers found that mice treated with LKM512-treated for 11 months lived longer, had fewer skin lesions, and had better hair quality than untreated mice. Another source describing the same study put it this way:
LKM512 administration downregulated [reduced/suppressed] the expression of aging-associated and inflammation-associated genes and gene expression levels in 21-month-old LKM512-treated mice such that they resembled those in 10-month-old untreated (younger) mice.
So, we know they lived 11 months longer than their brethren and they expressed biometrics usually found in mice half their age, but the actual lifespan achieved wasn’t mentioned.
Conclusion
Your Need the Right Gut Bacteria to Achieve A Healthy Firmicutes to Bacteroidetes Ratio
Firmicutes and Bacteroidetes are bacteria phyla. In humans, about 90% of gut bacteria are represented by these two phyla (a taxonomic classification).
Everyone’s gut has many billions, if not trillions, of each. But if you want all kinds of good, healthy things happening to you, the ratio to strive for is just below 50/50 in favor of Bacteroidetes; meaning, a bit more Bacteroidetes than Firmicutes. (Read more about this here.)
Salveo Diagnostics offers this interpretation of the F/B ratio:
| Low | Mildly Low | Optimal | Mildly High | High |
| ≤ 0.2 | 0.3 | 0.4 – 3.7 | 3.8 – 20.9 | ≥ 21.0 |
How do you get the right balance?
You must give those bugs the right food.
Conclusion
To Get The Right Gut Bacteria, Feed It Right
The good news — the foodstuff that’s good for your beneficial bacteria is good for you too!
For optimal balance of the gut microbiota, consider a diet low in refined carbohydrates and processed foods, rich in fiber, essential fatty acids, and phytonutrients, with a wide variety of fresh fruits and vegetables, beans (legumes), nuts, and whole grains.
I grabbed the following suggestions from my article, Test How Your Invisible Gut Bacteria Affects Your Health, which may help restore your microbiota:
- Specific pharmaceutical or botanical medications may be taken under the guidance of a qualified clinician for the treatment of bacterial, fungal, or parasitic infections.
- Abstinence from gut-damaging medications (e.g., antibiotics, nonsteroidal anti-inflammatory drugs, proton-pump inhibitors, oral contraceptives) and alcohol.
- Probiotics, especially Lactobacilli and Bifidobacteria, help restore GI balance; they activate anti-inflammatory pathways, regulate gut contractility and calm IBS symptoms, improve weight control and insulin sensitivity, and reinforce intestinal barrier integrity. “Reseeding” the dysbiotic gut with these friendly bacteria may preclude pathogens taking up residence. Probiotics can be found in fermented foods (e.g., yogurt, miso, tempeh, and sauerkraut) or taken as supplements.
- Prebiotics, food ingredients that feed the gut flora, can augment the benefits of probiotics and include bran, resistant starch, and oligosaccharide-containing foods such as onions, garlic, leeks, chicory, asparagus, tofu, and bananas. Supplemental prebiotics may help patients with low levels of beneficial short chain fatty acids.
- Low stomach acid (often resulting from treatment with gastric acid suppressants) and pancreatic insufficiency may exacerbate the effects of dysbiosis by impairing digestion and assimilation of food.4 If fecal elastase (a diagnostic test for pancreatic function) levels are low, consider supplemental pancreatic enzymes. Drinking warm water containing fresh lemon juice before meals may aid digestion by stimulating gastric acid secretion.
- Patients with dysbiosis may benefit from vitamin and mineral supplements to address associated nutrient deficiencies. The MegaFood brand is exceptional.
- Regular physical exercise lowers inflammation, and can increase microbial diversity and decrease transit time.
I wrote a post about Dr. Andrew Weil’s Anti-inflammation Diet. I called it, Why Dr. Weil’s Anti-Inflammation Pyramid May Be The Best Diet. Here’s what it looks like:

I’m telling you about this because an anti-inflammation diet is one that is highly beneficial to the right gut bacteria so necessary for your overall health.
The base of this anti-inflammation diet pyramid is loaded with fruits and veggies, the very foods that contain the wonderful, endotoxin ass-kickers, the prebiotic oligosaccharides.
You might wish to examine the pyramid and see what food categories are absent from your diet. I wouldn’t worry much if you’re not eating grains and pasta — they don’t have much nutritional value and some nutritionists believe that the gluten contained in them is responsible for various autoimmune diseases.
Specific foods you can begin to add to your diet that are inflammation fighters include:
- Garlic
- Ginger
- Curcumin
- Tumeric
- Keifer
- Sauerkraut
- Broccoli sprouts
- Asparagus
- Natto
- Kimchi
- And to ensure a steady supply, probiotic supplements.
If you’re interested in learning more about which foods best nourish the right gut bacteria, read two of my articles:
- uBiome’s 7 Secrets About How Some Gut Bacteria (Like Firmicutes) Can Make You Fat, and
- The 4 Food Solution to the 100 Trillion Reasons You’re Fat, Sick and Depressed.
Conclusion
Build the Right Gut Bacteria by Supplementing with Prebiotics and Probiotics
When it comes to feeding a healthy microbiome, you can’t go wrong with focusing on these three things, which I pulled from my article, How To Feed 100 Trillion Guests:
Probiotics are live microorganisms, or beneficial microbiota, that may confer a health benefit on the host (you). Yogurt has lots of these, kefir even more. You can also buy probiotic supplements.
Prebiotics are non-digestible food ingredients that stimulate the growth and/or activity of bacteria in the digestive system in a manner that may be beneficial to health. Fermented foods such as sauerkraut and kimchi have prebiotics. You can also buy prebiotic supplements.
Synbiotics refer to nutritional supplements combining probiotics and prebiotics in a form of synergism, hence “synbiotics”. You can buy synbiotics as supplements or eat foods containing probiotics and prebiotics, as mentioned above.
Dr. David Williams is a globe-trotting medical researcher, biochemist, chiropractor, and leading authority on natural health . He believes that the probiotics Bifidobacterium and Lactobacillus show beneficial effects on anxiety and depression-like behavior, but only in specific strains:
- Bifidobacterium infantis improved early-life stress-induced immune changes and depressive-like behaviors in adulthood. See PB8 Probiotic on Amazon.com
- Lactobacillus helveticus ROO52 has also been shown to reduce anxiety-like behavior and alleviate memory dysfunction. See Garden of Life Probiotic on Amazon.com
- Lactobacillus rhamnosus JB-1 reduced anxiety- and depression-related behaviors in the elevated plus maze and forced swim test, respectively. See Nexabiotic Advanced Probiotic on Amazon.com
- Mycobacterium vaccae reduced anxiety and improved performance on a complex maze task
- Bifidobacterium longum normalizes anxiety-like behavior in a colitis (inflammation of the inner lining of the colon) model. See Nexabiotic Advanced Probiotic on Amazon.com
I got your head spinning again, yes? Mine too.
What do you do with this information?
If any of the strains described above address your health concern, click on the Amazon link and see if the probiotic product(s) may be for you.
You may also check out Labdoor’s Top 10 laboratory tested and rated probiotics.
Lastly, read my article Heal Yourself and Become Superman with Specialized Probiotics where I delve into the foods to eat that feed your beneficial bacteria and list the probiotic strains favored by Dr. David Williams, which are:
- L. acidophilus—This is the most important strain of the Lactobacillus species and, it readily colonizes on the walls of the small intestine. It supports nutrient absorption and helps with the digestion of dairy foods.
- B. longum—Like L. acidophilus, B. Longum is one of the most common bacteria found in the digestive tracts of adults, and it helps maintain the integrity of the gut wall. It is particularly active as a scavenger of toxins.
- B. bifidum—This strain, found in both the small and large intestine, is critical for the healthy digestion of dairy products. This is especially important as you grow older and your natural ability to digest dairy declines. B. bifidum also is important for its ability to break down complex carbohydrates, fat, and protein into small components that the body can use more efficiently.
Secondarily, Dr. Williams likes:
- L. rhamnosus—Known as the premier “travel probiotic,” this strain can help prevent occasional traveler’s diarrhea.
- L. fermentum—This Lactobacillus strain helps neutralize some of the byproducts of digestion and promote a healthy level of gut bacteria.
This is Dr. William’s formulated probiotic product:
There’s also a Life Extension Foundation supplement containing probiotics known to positively influence biochemical signaling between the gastrointestinal tract and the nervous system, with positive effects on mood, called FLORASSIST® Mood. The two bacterial strains are Lactobacillus helveticus strain R0052 and Bifidobacterium longum strain R0175. I haven’t used it, can’t vouch for it, but you may wish to learn more about it.
Conclusion
The Right Gut Bacteria Is Killed By Antibiotics
Yes, you know this already, but at long last we need circle back to my friend, Dara, ailing with that infection I mentioned.
What I didn’t say is that the infection that brought her to her knees was a couple of feet north of them — her urinary tract.
Yes, the dreaded UTI.
And before you males exit at this point, remember that you have mothers, daughters, wives, girlfriends (hopefully not both) and perhaps (as I was lucky enough to have till the age of 50), grandmothers.
They all need to know about this, and you fellas can be their heroes for passing along this information, cause the facts are that:
- About 50 to 60 percent of adult women have had at least one UTI. (1)
- Urinary Tract Infections are the second most common type of infection that people get, accounting for 8.3 million doctor visits every year in the United States. (2)
- About one in five women will get a recurrent UTI, and women who have more than three UTIs are more likely to continue having them. (2)
When you go to a doctor to treat a UTI, or basically any other bacterial infection, what do you get? Yes, antibiotics. You take them, and what do you get? Yes, dead gut bacteria. You kill your gut bacteria, and which ones tend to recover more quickly (unless you’re very diligent with diet and supplementation)? Yes, the wrong bacteria that amps up inflammation and weight gain and taps down cognitive function and your immune system.
So, what to do?
5 Natural Antibiotics
The good news is that there are many natural antibiotics that work equal to or better than antibiotic drugs. If you were to google “natural antibiotics” you’d get various long lists, each containing many of the same candidates.
These are my five favorite natural antibiotics:
(1) D-mannose — Similar to glucose in structure, D-mannose is a naturally occurring sugar that is found in a number of fruits, including apples, blueberries, and cranberries. This is the one that Dara took, and as reported, it quickly eased her symptoms and got rid of her UTI just as quickly as the antibiotic drugs could.
Despite being a type of sugar, D-mannose does not cause any adverse side effects, even in large quantities, as it’s not metabolized like other sugars, and thereby doesn’t destroy beneficial gut bacteria, nor is it dangerous for diabetics.
The typical dose of D-mannose for UTI treatment is 500 mg, in capsule or powder form, taken in a glass of water or juice every two to three hours for five days. Continue taking the supplement even after symptoms have diminished to ensure complete elimination of the bacteria in the urinary tract. This dose can also be taken as a preventative, or prophylactic method. (3)
Dr. Joe Mercola has a propreitary D-mannose product you may consider, called, well, D-Mannose.
(2) Garlic Extract — Long considered to have antimicrobial properties, a 2011 study pretty much proved it to be so, as it found that garlic concentrate is effective against bacteria. You can purchase garlic concentrate or extract at your local health food store.
It may seem nuts, but when I feel some sorta illness knocking at my door, I crush up about eight raw cloves and lather them on toast with almond butter. Yes, I actually can eat this:
Garlic is generally safe to ingest, but large doses might cause internal bleeding. Up to two cloves per day is considered an acceptable dosage, although as mentioned I’ve worked my way up to multiples of that. If you’re taking a garlic supplement, be sure to follow the dosage directions as provided.
You can apply garlic concentrate directly to a wound or blemish. If you’re taking blood-thinning medication, consult your doctor before using garlic as an antibiotic. Large doses of garlic can amplify the effects of this medication. (4)
If you rather not chew the raw stuff, consider a garlic supplement. This one is very highly rated on Amazon.
(3) Oregano Oil — Wild oregano oil (Origanum vulgare) has a high antibiotic power that can help to fight different types of microorganisms. This type of oil is a red or dark yellow color, with a strong spicy smell.
- Fungus in the toes or nails: Add a couple of teaspoons of oregano oil in a tub with hot water and soak your feet for 10 minutes. Another option is to mix a drop of this oil with a teaspoon of olive oil and then apply it directly to the toes and nails.
- Parasites and infections: Mix a drop of this oil with a teaspoon of olive oil and put it under your tongue. Keep it there for a minute and then rinse your mouth out. Repeat this four times a day.
- Sinusitis: Place a few drops of oregano oil in a pan with boiling water and breathe the steam.
(4) Tea Tree Oil — Another strong natural antibiotic, tea tree oil has antibacterial, anti-fungal and anti-inflammatory properties. Derived from the leaves of the tea tree, it’s topically used on skin to prevent skin plaque, redness, acne and pimples.
Tea tree oil is one of the best Ayurvedic natural antibiotic as it has over 45 modern medicine applications. It can cure fungus infections of the nails (onychomycosis). Topical application of 100% tea tree oil solution, twice daily for six months, can cure fungal toenail infection in about 18% of people who try it. It can also improve nail appearance and symptoms in about 56% of patients after three months and 60% of patients after six months of treatment. (5)
I use the the Trader Joe’s brand from my local grocer. I dab some on any rash or wart that has the temerity to think they’re gonna mess with me.
(5) Grapefruit Seed Extract — Famous due to its ability to kill microbes and fungal infections, grapefruit seed extract uses are numerous due to its action as a highly concentrated, natural general antimicrobial and antioxidant. Grapefruit is a citrus fruit, a source of vitamin C, fiber, potassium, and other nutrients. People use the fruit, oil from the peel, and extracts from the seed as medicine. (5)
Although I think it’s great, it has a very strong, unpleasant taste. I use a few drop of a grapefruit extract in water when I’m about to get exposed to microbes that I might not have some immunity to, such as when I travel. Alternatively, you can use tablets.
I’ve used all five these five natural antibiotics and believe they’re a better alternative to antibiotic drugs; moreover, each of these five are actually healthy for you.
Conclusion
Your Takeaway
Remember these four things:
- Antibiotic drugs are so prevalent in the world today that they threaten their own capacity to work against the ever increasing capacity of drug resistant microbes.
- Many natural antibiotic supplements are as good or better than the pharmaceutical varieties, particularly when you consider the beneficial effects the natural antibiotics have upon your beneficial gut bacteria.
- The bacteria in your gut — part of your overall microbiome — strongly affects your health in numerous ways, and its impact on body composition, chronic inflammation, metabolism, immunity, cognition and longevity.
- An anti-inflammation diet combined with pre and probiotic supplementation has an immense, favorable impact on supporting your beneficial bacteria, which then contributes mightily to all the good things cited in #3 above.
I salute your healthy bugs!
Last Updated on June 21, 2022 by Joe Garma