Women’s Hormone Replacement Therapy: What You Need to Know

Women’s hormone replacement therapy, if done right, can substantially improve health outcomes. Unfortunately, one poorly conducted study in particular has dissuaded women from such therapy. Here’s enough to know to ask your doctor about it.
⦿ Women's hormone replacement therapy consisting of estrogen, progesterone and testosterone can improve health outcomes. ⦿ The ratio of 1-to-1 between estrogen and progesterone is important to maintain post menopause. ⦿ Men need to do what they can to boost testosterone as they age, either via bio-identical therapy or naturally.
Women’s hormone replacement therapy (HRT) has long been a crucial aspect of women’s healthcare, particularly for those going through menopause. In this review, I want to provide valuable insights into the various aspects of hormone replacement for women (primarily), with the aim of provoking awareness of about its benefits, given that historically it’s been given some deep shade.
But there is a disclaimer that must attend this information:
Because our endocrine system influences nearly every aspect of our biology, it’s wise to practice an abundance of caution when considering self-administered hormone therapy. Given the profound impact hormones can have on one’s health, it’s strongly advised to seek the counsel of an endocrinologist or healthcare professional well-versed in this field. Their expertise can help ensure that any hormone replacement therapy is tailored to your unique needs.
In this post, we will delve into the world of women’s hormone replacement therapy, and discuss estrogen therapy, centered on estrogen, progesterone and testosterone. Speaking of testosterone, I will give the men their due as well.
OK, let’s dig in…
Introduction to Hormone Replacement Therapy
HRT, or Hormone Replacement Therapy, is a medical approach aimed at supplementing or replacing hormones that the body no longer produces in sufficient quantities.
In the context of women’s health, HRT is predominantly used during menopause, a natural biological process that marks the end of a woman’s reproductive years.
Menopause typically occurs in a woman’s late 40s or early 50s, and it brings about a significant hormonal shift, particularly a decline in estrogen levels, which is characteristic of menopause. The use of estrogen replacement therapy has been a longstanding approach to manage the symptoms associated with menopause. These symptoms include hot flashes, night sweats, vaginal dryness, and concerns related to bone health.
Let’s flesh out the rest of this introduction to HRT with a discussion on the topic between clinician and longevity expert Peter Attia, MD, and Stanford neuroscientist Dr. Andrew Huberman. In the video below, Dr. Huberman asks Dr. Attia about what he thinks of HRT and to what extent he uses this in his practice.
Women’s Hormone Replacement Therapy: the Big 3
Hormones are vital chemical messengers that regulate various bodily functions, and during menopause, imbalances in key hormones can lead to distressing symptoms. In HRT, the three primary hormones involved are:
- Estrogen,
- Progesterone and
- Testosterone
Let’s touch on each.
Estrogen
Estrogen is the primary female sex hormone responsible for maintaining various physiological processes in a woman’s body, including menstrual cycles, bone health, and the health of the female reproductive system.
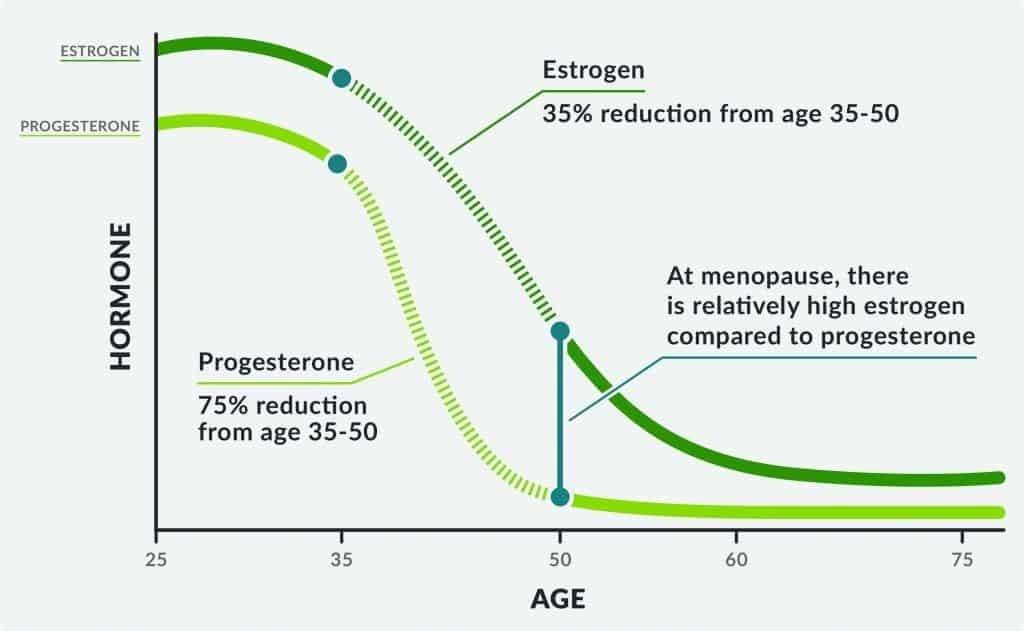
During menopause, a woman’s estrogen levels significantly decline, leading to symptoms like hot flashes, night sweats, and vaginal dryness. Estrogen replacement therapy has been a longstanding approach to manage these symptoms, as well as to concerns related to bone health. However, after menopause, the levels of both estrogen and progesterone decrease, and the ratio between them changes.
The levels of estrogen decrease more than the levels of progesterone, leading to a higher ratio of progesterone to estrogen. This shift in the ratio can lead to an increased risk of endometrial cancer, which is why it’s essential to monitor hormone replacement therapy through endometrial ultrasounds to ensure that the treatment remains both safe and effective.
The use of bioidentical hormones, such as estradiol and micronized progesterone, can help maintain a healthy balance of hormones and reduce the risk of endometrial cancer. It’s crucial to tailor hormone replacement therapy to meet each woman’s unique needs, and regular monitoring is key to its success.
Progesterone
For women who have a uterus, the use of estrogen alone can increase the risk of uterine cancer. Thus, in combination with estrogen therapy, progesterone is often prescribed. To repeat: Progesterone helps counteract the estrogen’s effects on the uterine lining, reducing the risk of endometrial cancer.
After menopause, the ratio between estrogen and progesterone typically changes. During menopause, the desired ratio between estrogen and progesterone for women is 1 to 1. However, after menopause, the levels of both hormones decrease, and the ratio between them changes. The levels of estrogen decrease more than the levels of progesterone, leading to a higher ratio of progesterone to estrogen.
This shift in the ratio can lead to an increased risk of endometrial cancer, which is why it’s essential to monitor hormone replacement therapy through endometrial ultrasounds to ensure that the treatment remains both safe and effective. The use of bioidentical hormones, such as estradiol and micronized progesterone, can help maintain a healthy balance of hormones and reduce the risk of endometrial cancer. It’s crucial to tailor hormone replacement therapy to meet each woman’s unique needs, and regular monitoring is key to its success.
Testosterone
While testosterone is often associated with male health, it’s intriguing to note that women also have testosterone in their bodies.
In fact, when you normalize the measurements, women can have more testosterone than estrogen. A normalized scale is a way of comparing measurements that takes into account the natural variations in the levels of hormones in the body. In the case of testosterone and estrogen levels in women, a normalized scale means that the levels of these hormones are compared on a scale that takes into account the natural variations in the levels of these hormones in women’s bodies.
Testosterone is important to postmenopausal women because it plays a role in maintaining muscle mass, bone density, and libido. If needed, the administration of physiologic testosterone in women rarely leads to symptoms like acne or excessive body hair growth. Instead, it may offer benefits such as improved muscle mass and libido.
Just like with the balance between estrogen and progesterone, the balance between estrogen and testosterone plays a significant role in women’s health. While estrogen therapy has been the primary focus, testosterone therapy for women is a relatively newer concept. When prescribed, it should be administered with caution, closely monitored, and maintained at levels that mimic physiological normality.
The Goals of Women’s Hormone Replacement Therapy
Hormone Replacement Therapy serves multiple purposes for women experiencing the symptoms of menopause, which can be categorized into two buckets: symptom relief and preventative health.
Symptom Relief
HRT is primarily used to alleviate the uncomfortable symptoms associated with menopause, such as hot flashes, night sweats, mood swings, and vaginal dryness. These symptoms can significantly affect a woman’s quality of life, and HRT can provide relief.
Preventive Health
HRT may have some preventive health benefits. It is believed to help maintain bone density, reducing the risk of osteoporosis and fractures. Some studies also suggest that HRT may reduce the risk of cardiovascular disease and colon cancer.
If you’re wondering if you might need HRT, check out this Hormone Questionnaire designed by third-generation endocrinologist Dr. Thierry Hertoghe. It will give you insight about any hormone imbalances you may have, which is very common as we age. You can optimize your hormones, but first you need to identify the problem areas.
Types of Hormone Replacement Therapy
There are various forms of women’s hormone replacement therapy, and the choice depends on the individual’s needs and preferences.
Oral Hormones
Hormones can be administered orally in the form of pills or tablets. However, this method may have a higher risk of side effects, such as blood clots and liver problems.
Transdermal Hormones
Hormones can be delivered through the skin via patches or gels. Transdermal HRT may offer a lower risk of certain side effects and allows for steady hormone release.
Topical Creams
Creams or gels can be applied topically to the skin, providing a localized effect.
Intrauterine Devices (IUDs)
Some women may opt for an IUD that releases hormones to provide localized relief, particularly for the management of symptoms like heavy menstrual bleeding and cramps.
For further reading on this topic, I suggest the following posts that I’ve written:
Bio-identical Hormone Replacement Therapy Is Simple — Just Follow Mother Nature’s Recipe: If you’ve wondered about the value of Bio-identical Hormone Replacement Therapy, you need to know about the estrodial/progesterone balance, the best way to take it, and how to test for hormone levels.
How Russell Crowe’s Makeup Artist Got To Look Fabulous With Hormone Therapy For Anti-aging: What is hormone therapy for anti-aging? Should you care about it? Hormone expert Dr. Paziotopoulos explains things to host to WGN-TV host Jane Monzures. And then Russell Crowe’s makeup artist shares how she became “the hottest mother of four he’s ever seen!”
The Negative Perception of HRT 
One pivotal event in the history of HRT for women is the Women’s Health Initiative (WHI) study. This study had a profound impact on the perception of hormone replacement therapy, and it’s essential to understand its context.
But was it flawed?
The WHI study is widely regarded as flawed due to various reasons. One notable issue was that the study participants were well beyond the typical age at which women begin HRT. Additionally, the WHI used synthetic hormones, specifically conjugated equine estrogen and synthetic progesterone (medroxyprogesterone acetate or MPA), which differ significantly from bioidentical hormones used today.
The flawed design of the WHI study and the use of these synthetic hormones contributed to misconceptions and fear surrounding HRT. It’s safe to say that this study has been one of the biggest sources of confusion in the field of women’s health over the past few decades.
A Glimpse into Testosterone Therapy for Men
While our primary focus in this post has been on women’s hormone replacement therapy, let’s not ignore the men.
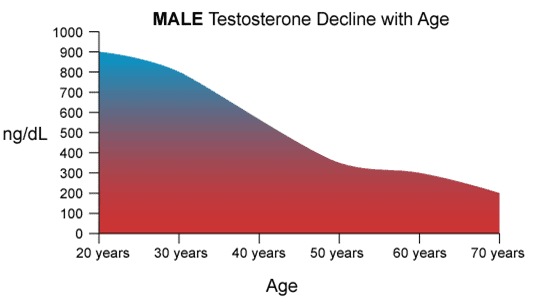
As men age, their testosterone declines:
An adequate level of testosterone is essential for men as they age because testosterone plays a crucial role in maintaining muscle mass, bone density, and libido.
As men age, their testosterone levels naturally decline, leading to a condition called andropause. Andropause is characterized by symptoms such as decreased energy levels, decreased muscle mass, and decreased libido. Testosterone replacement therapy can help address these symptoms and improve overall well-being.
The desired level of testosterone for men varies depending on age and other factors, but a general guideline is that men should have testosterone levels between 300 and 1000 ng/dL.
Bio-identical Testosterone Hormone Therapy for Men
Several of my male middle aged friends and beyond use identical testosterone therapy, either applying a gel once a day to their body, or self-administering a shot once a week or so.
They’re being smart about it; meaning, they’re not trying to overdo the dose in some vain attempt to strut around like a bodybuilder, and they’re under a doctor’s care who monitors blood work twice a year.
And it’s working for them — these fellas are living full, energetic lives, although I need to underscore that the extra testosterone kick isn’t entirely responsible for this, given that everyone who comes to mind in this regard is also eating healthily and exercising consistently.
All that said, there are downsides to this testosterone HRT, including:
- Gonad testosterone production: Testosterone replacement therapy can lead to a decrease in the production of testosterone by the testes, leading to testicular atrophy. This can result in a decrease in sperm production and fertility.
- Prostate cancer: Testosterone replacement therapy can increase the risk of prostate cancer. However, the evidence is mixed, and more research is needed to fully understand the relationship between testosterone therapy and prostate cancer.
- Cardiovascular disease: Testosterone replacement therapy can increase the risk of cardiovascular disease, including heart attacks and strokes. However, the evidence is mixed, and more research is needed to fully understand the relationship between testosterone therapy and cardiovascular disease.
- Acne and hair loss: Testosterone replacement therapy can lead to acne and hair loss in some men.
- Sleep apnea: Testosterone replacement therapy can worsen sleep apnea, a condition in which breathing stops and starts during sleep.
Given the potential downsides of using bio-identical testosterone, I underscore again that It’s essential to be closely monitored by healthcare providers.
In my case, I opt for “natural” boosts to my testosterone.
Testosterone-boosting Supplements and Exercise
I’ve written quite a bit about how to naturally boost a man’s testosterone levels, and that reflects what I do, which I’ll turn to in a moment.
The reason I rely on “natural” testosterone-boosting methods is simply because:
- The natural approach seems to be working — I’m maintaining muscle and energy, and
- I want my boys (gonads) to keep in fine operational order.
Nearly ten years ago when I was in my late 50s, I had my testosterone checked and it was in the high 400s (ng/dL). I finally got it checked again last month and it was in the high 500s (ng/dL) — not bad for a decade later.
Now, mind you, the absolute testosterone number isn’t as important as what’s circulating, the so-called “free testosterone” (I increased that as well over the past decade), and different men respond differently to a particular level. What I mean is that I may do well with a total T of 500, but another man might need more or less. This tends to be highly variable and personal.
As I tend to do, I experiment with various testosterone-boosting methods, which you can read about by clicking the links to any of these posts:
8 Testosterone Enhancing Supplements (and 2 drugs) That Will Keep You From Turning Into A Girl: These eight testosterone enhancing supplements and two drugs might just be what you need to generate more vim and vigor (among other things). But, men, beware estradiol. And women, you need testosterone, too.
Boost Your Testosterone The Natural Way: Here’s How: Fellas, once you pass 40, there’s few things you can do for yourself that will feel better than to boost your testosterone, cause — odds are — your testosterone number is too low. Learn how to do it the natural way. Or the other way.
How I’m Boosting Testosterone and Blasting Body Fat: Your testosterone is low and body fat’s high. It often works that way. Improve one and the other improves too. This post details what I’m doing to measure and manage nutritional inputs as I endeavor to boost my testosterone and blast away some body fat.
Your Takeaway
Women’s hormone replacement therapy can play a crucial role in women’s health, particularly for those going through menopause.
An HRT program that balances estrogen and progesterone, while also keeping tabs on testosterone can help alleviate menopausal symptoms and improve overall well being.
Testosterone therapy for women remains a topic of ongoing research, with the need for caution and personalized treatment plans. But testosterone therapy clearly is something that men may choose to undertake, whether via bioidentical hormone or doing it the “natural” way as I outlined above.
Understanding the nuances of hormone replacement therapy is essential, and that means that you need a health professional to help you regularly monitor your levels in order to be confident that you’re getting what you need without harming yourself.
Last Updated on November 9, 2023 by Joe Garma