How Your Thyroid Ignites Chronic Health Problems, Part 2
You may have no reason to think about your thyroid, but whatever health issue is bullying you, here you’ll learn something about how to tackle and take it down.
WHEN YOU break a leg it’s not your arm’s fault. I mean, the health of your arm had nothing to do with your leg breaking. There’s something comforting in that. Break a leg, put on a cast, let it heal, nothing else is involved.
But if some set of behaviors or conditions or your genetics disrupts the proper functioning of your hormones, a complicated, interrelated cascade of physical and mental/emotional disruptions erupt.
They could hit you fast and hard, or come on slowly like a tub’s dripping faucet that eventually overflows.
Either way, the result is the same… your health becomes compromised, and thus your life.
Eight months ago I wrote The Poor Performing Hormone That May Cause Your Chronic Health Problems, Part 1, and now, finally, I’m prepared to offer you Part 2.
Part 1 explored the riddle that many of us face. It’s a mysterious trip we take when everything seems fine on the surface, but you discover something pernicious brewing within.
You may look in the mirror and see a robust person looking back. All seems good enough. But you have some indication that something’s amiss. Perhaps your energy is consistently flagging, or you feel depressed. Maybe you got a blood test and several health “markers” indicate there’s a problem.
And you wonder how it all connects.
In Part 1, I led readers through a labyrinth.
There was a mystery to solve.
I established that there may be a causal or connected factor behind a myriad of disquieting blood health markers, such as:
- Testosterone (and other “sterones“),
- Serum Glucose (blood sugar),
- Homocystin (cardiovascular health),
- VLDL (Very-low-density lipoprotein cholesterol, a marker for coronary artery disease)
- C-Reactive Protein (inflammation marker), and
- TSH (Thyroid Stimulating Hormone, a marker for thyroid function).
Collectively, my blood results for the above listed “markers” indicated that something’s amiss, that my health isn’t as hale as one would think by observing me scurrying about, eating all that heath food, twisting around with yoga, sprinting stairs and lifting weights.
Therein lies the mystery. One that needs to unravel before your very eyes. Then you take what you learn and apply it to whatever may be your own health mystery.
The null hypothesis I established in Part 1 still remains to be disproved, and it is this:
I have hypothyroidism — low functioning thyroid — and it is causing some, if not all, of the other health issues indicated by my blood test.
Today I received in the mail the “supplement” that will kick start Part 3 of my protocol to boost my thyroid function and thereby (presumably) improve those health markers listed above.
It seems reasonable that before I begin Part 3’s journey, I tell you what happened in Part 2. That’s here and right now. In this article, I’ll share what I’ve learned these last eight months with the aim to support or discredit my hypothesis.
Least you think this mysterious journey is all about me… well, it is and it isn’t.
I’m merely the example.
The value to you is to glean whatever is useful and apply it wherever it may work.
If you’re consistently feeling rundown and tired, are overweight and can’t seem to lose the extra jiggly, are moody, or darn near depressed… could be that you need to tweak your hormones.
They’re slippery things, those hormones and esquisitely interconnected. You’ll need to take measured steps, test and retest, and sometimes fail.
In this article, you’ll learn:
- Why my null hypothesis is that I have hypothyroidism;
- How different biochemical mechanisms and reactions affect your thyroid, and one another; and
- What I’m doing to combat my hypothyroidism.
Why I May Have Hypothyroidism (do you?)
Even if it’s not you, you probably know someone with low functioning thyroid.
Millions of people in the USA have this condition. I could list the symptoms but they’re nearly the same for adrenal fatigue and other hormone deficiencies, so they wouldn’t pinpoint a thyroid issue without further dissection.
(If you really want a list, go here and scroll down to”Dr. Lam’s Chart”.)
Basically, hypothyroidism happens when the thyroid gland becomes under-active, failing to sufficiently secrete the hormones that help convert food and oxygen into energy.
Frankly, I’m not 100% sure I have hypothyroidism, and if I do, I have no idea if it’s caused by an autoimmune disease (which would make it Hashimoto’s).
My sister has hypothyroidism and it’s been diagnosed as being part of an autoimmune issue that may be instigated by a gluten allergy. (Isn’t everything caused by gluten these days?)
My mother has been diagnosed with hypothyroidism, but I don’t think the blood test was very thorough.
The only blood work I’ve done directly pertinent to the thyroid is the Thyroid Stimulating Hormone (“TSH”) test, which is insufficient to diagnose a thyroid problem. As I wrote in The Poor Performing Hormone That May Cause Your Chronic Health Problems:
TSH rises when the thyroid is under active because the pituitary gland is releasing more hormone to try to get the thyroid to respond and produce more thyroid hormone.
If the pituitary senses that there’s too much thyroid hormone circulating, it slows down or even stops releasing TSH, which means the thyroid is no longer getting the message to release hormone, and thyroid hormone production will slow down.
So, TSH responds inversely to thyroid hormone production — it (TSH) goes up when your thyroid hormone goes down and visa versa.
A TSH below 0.3 mIU/L is indicative of hyperthyroidism (thyroid produces too much thyroid hormone) and above 3.0 is indicative of hypothyroidism (produces too little).
My TSH number is 3.07. That’s not much above the range, but enough to have put me into action to find out what’s up.
And what’s up includes a few more symptoms that point to hypothyroidism, such as:
- My feet were cold
- My Achilles tendon was sore
- My eyebrows have thinned
- I get tired and listless too often
- My body temperature is way low
Let’s briefly look at each of these…
Cold Feet
It makes sense that if a hormone that is responsible for converting food and oxygen into energy is under-performing, you get cold. The most noticeable places this happens is at your hands and feet.
For me it’s primarily my feet, and the only time I really noticed it was in bed. Sometimes, they’d feel so cold that I couldn’t fall asleep. Rubbing them together didn’t help. Socks didn’t help. Strangely, putting on warm pajama bottoms did.
Well, anyway, my feet “were” cold and now they’re not, mostly. The cold feet went away once I began taking Thytrophin.
Sore Tendon
This one took me by surprise.
About a 100 years ago when I was in my mid-thirties I was playing basketball one fine day. Dribbling at the top of the key, I feigned left, spun right and charged to the basket.
Just as I sprung off my left foot I heard a pop.
I don’t know if this happens to everyone else, but when my Achilles tendon ruptured, it made a popping sound.
I spend two days hobbling around pretending that this was just another badly sprained ankle, as if I didn’t know basic anatomy. Surgery reattached things and after some more hobbling around I was fine, and that Achilles tendon in my left leg never troubled me again.
Not so it’s brother, Mr. Right Tendon.
The right Achilles tendon would get sore whenever I ran or jumped too much.
About a year ago, I began sprinting stairs for my high intensity interval training, a sure-fired way to get fit, lean and produce more human growth hormone. Sure enough, after awhile, my Achilles on my right leg got sore.
No more stairs and a limping walk were the result.
I was frustrated and wondered if I was trying too hard to act like a young man. But then I bumped into an article on the Interwebs, and it said that hypothyroidism can cause soreness in tendons. I can’t find the article, but at the time I felt it could be true.
My Achilles tendon is no longer sore, and that — like the cold feet — I think is the result of taking Thytrophin. (More about Thytrophin later.)
Thin Eyebrows
I have no idea why, but thinning eyebrows can be an indication of hypothyroidism. Even Drs. Oz and Roisen think so. They suggest this test:
“Stand in front of a mirror. Hold a pencil up to the outer corner of your left eye, so that the pencil is vertical — one end points to the floor, the other to the ceiling. Check to see if there’s eyebrow hair to the left of the pencil. One sign of low thyroid is the loss of eyebrow hair here (not because you plucked or waxed it off, of course!). If you’re hairless there, check the symptom list again, and talk with your doc.” (Source)
Here’s one of mine, which looks even more sparse that the pic depicts:
Tired and Listless
If you’re tired, listless, a bit depressed… you can look nearly everywhere for the reason(s) why.
On the list put adrenal fatigue, low testosterone (men), perimenopause (uh, that would be women), chronic stress, too little sleep, metabolic syndrome, etc., etc.
Hypothyroidism is on the list as well, and this is yet another reason why I think I have it — I’m tired and listless too often, in my opinion.
Low Body Temperature
Last, but by no means least, is low body temperature.
Other than blood tests, your body temperature is probably the most predictive measure of hypothyroidism.
In the morning before you get out of bed, put an old fashioned thermometer (the kind you shake) under your arm pit, at about a 45 degree angle, for 10 minutes and see what it indicates.
Anywhere between 98.2 and 97.2 Fahrenheit is considered normal.
Over the course of seven months, mine only got above 97 thrice. Mostly, the readings clustered between 95 and 96, thereby indicating low functioning thyroid.
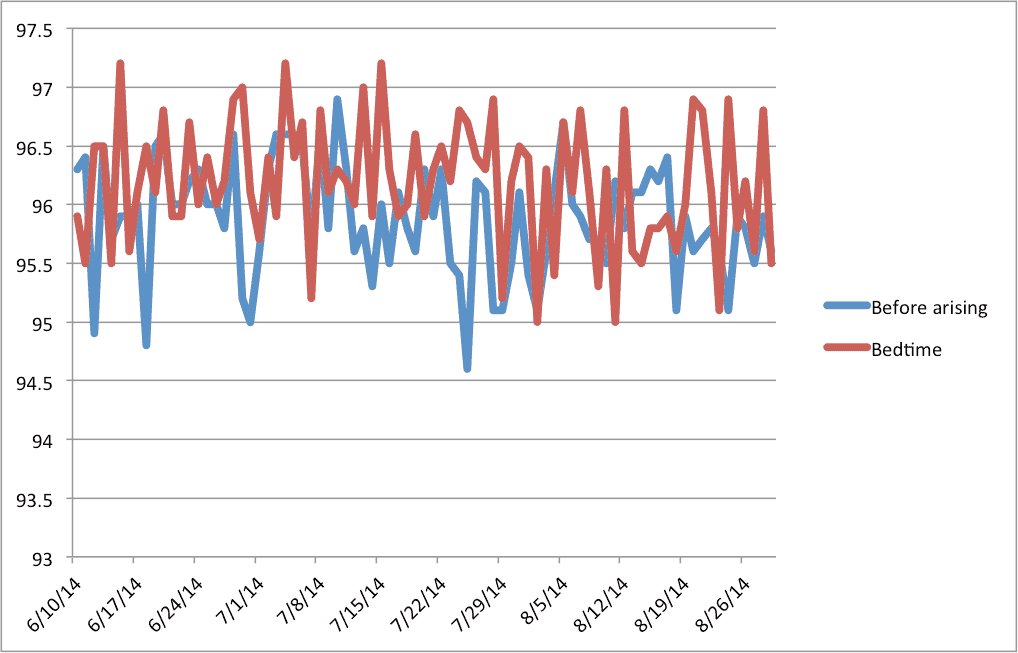
Here’s the graph showing two temperature readings per day, before arising and before sleeping, over the course of three months:
Joe’s Body Temperature Over Time
Click to see data
| Before arising | Bedtime | Thytrophin tablets | Thytrophin mg | |
| 6/10/14 | 96.3 | 95.9 | 3 | 327 |
| 6/11/14 | 96.4 | 95.5 | 3 | 327 |
| 6/12/14 | 94.9 | 96.5 | 3 | 327 |
| 6/13/14 | 96.5 | 96.5 | 3 | 327 |
| 6/14/14 | 95.7 | 95.5 | 3 | 327 |
| 6/15/14 | 95.9 | 97.2 | 3 | 327 |
| 6/16/14 | 95.9 | 95.6 | 3 | 327 |
| 6/17/14 | 96 | 96.1 | 3 | 327 |
| 6/18/14 | 94.8 | 96.5 | 3 | 327 |
| 6/19/14 | 96.5 | 96.1 | 3 | 327 |
| 6/20/14 | 96.6 | 96.8 | 3 | 327 |
| 6/21/14 | 96 | 95.9 | 0 | 0 |
| 6/22/14 | 96 | 95.9 | 0 | 0 |
| 6/23/14 | 96.2 | 96.7 | 4 | 436 |
| 6/24/14 | 96.3 | 96 | 4 | 436 |
| 6/25/14 | 96 | 96.4 | 4 | 436 |
| 6/26/14 | 96 | 96 | 4 | 436 |
| 6/27/14 | 95.8 | 96.2 | 4 | 436 |
| 6/28/14 | 96.6 | 96.9 | 4 | 436 |
| 6/29/14 | 95.2 | 97 | 4 | 436 |
| 6/30/14 | 95 | 96.1 | 4 | 436 |
| 7/1/14 | 95.6 | 95.7 | 4 | 436 |
| 7/2/14 | 96.3 | 96.4 | 5 | 545 |
| 7/3/14 | 96.6 | 95.9 | 5 | 545 |
| 7/4/14 | 96.6 | 97.2 | 5 | 545 |
| 7/5/14 | 96.6 | 96.4 | 5 | 545 |
| 7/6/14 | 96.5 | 96.7 | 5 | 545 |
| 7/7/14 | 95.7 | 95.2 | 5 | 545 |
| 7/8/14 | 96.6 | 96.8 | 5 | 545 |
| 7/9/14 | 95.8 | 96.1 | 5 | 545 |
| 7/10/14 | 96.9 | 96.3 | 5 | 545 |
| 7/11/14 | 96.3 | 96.2 | 5 | 545 |
| 7/12/14 | 95.6 | 96 | 5 | 545 |
| 7/13/14 | 95.8 | 97 | 5 | 545 |
| 7/14/14 | 95.3 | 95.9 | 5 | 545 |
| 7/15/14 | 96 | 97.2 | 5 | 545 |
| 7/16/14 | 95.5 | 96.3 | 5 | 545 |
| 7/17/14 | 96.1 | 95.9 | 5 | 545 |
| 7/18/14 | 95.8 | 96 | 5 | 545 |
| 7/19/14 | 95.6 | 96.6 | 5 | 545 |
| 7/20/14 | 96.3 | 95.9 | 5 | 545 |
| 7/21/14 | 95.9 | 96.3 | 5 | 545 |
| 7/22/14 | 96.3 | 96.5 | 5 | 545 |
| 7/23/14 | 95.5 | 96.2 | 5 | 545 |
| 7/24/14 | 95.4 | 96.8 | 5 | 545 |
| 7/25/14 | 94.6 | 96.7 | 5 | 545 |
| 7/26/14 | 96.2 | 96.4 | 5 | 545 |
| 7/27/14 | 96.1 | 96.3 | 5 | 545 |
| 7/28/14 | 95.1 | 96.9 | 5 | 545 |
| 7/29/14 | 95.1 | 95.2 | 5 | 545 |
| 7/30/14 | 95.5 | 96.2 | 5 | 545 |
| 7/31/14 | 96.1 | 96.5 | 5 | 545 |
| 8/1/14 | 95.4 | 96.4 | 5 | 545 |
| 8/2/14 | 95.1 | 95 | 5 | 545 |
| 8/3/14 | 95.6 | 96.3 | 4 | 436 |
| 8/4/14 | 96.1 | 95.4 | 5 | 545 |
| 8/5/14 | 96.7 | 96.7 | 2 | 218 |
| 8/6/14 | 96 | 96.1 | 2 | 218 |
| 8/7/14 | 95.9 | 96.8 | 2 | 218 |
| 8/8/14 | 95.7 | 96.1 | 2 | 218 |
| 8/9/14 | 95.7 | 95.3 | 2 | 218 |
| 8/10/14 | 95.5 | 96.3 | 2 | 218 |
| 8/11/14 | 96.2 | 95 | 2 | 218 |
| 8/12/14 | 95.8 | 96.8 | 2 | 218 |
| 8/13/14 | 96.1 | 95.6 | 2 | 218 |
| 8/14/14 | 96.1 | 95.5 | 2 | 218 |
| 8/15/14 | 96.3 | 95.8 | 2 | 218 |
| 8/16/14 | 96.2 | 95.8 | 2 | 218 |
| 8/17/14 | 96.4 | 95.9 | 2 | 218 |
| 8/18/14 | 95.1 | 95.6 | 2 | 218 |
| 8/19/14 | 95.9 | 96 | 2 | 218 |
| 8/20/14 | 95.6 | 96.9 | 2 | 218 |
| 8/21/14 | 95.7 | 96.8 | 2 | 218 |
| 8/22/14 | 95.8 | 96.1 | 2 | 218 |
| 8/23/14 | 95.6 | 95.1 | 2 | 218 |
| 8/24/14 | 95.1 | 96.9 | 2 | 218 |
| 8/25/14 | 95.9 | 95.8 | 2 | 218 |
| 8/26/14 | 95.8 | 96.2 | 2 | 218 |
| 8/27/14 | 95.5 | 95.6 | 2 | 218 |
| 8/28/14 | 95.9 | 96.8 | 2 | 218 |
| 8/29/14 | 95.6 | 95.5 | 2 | 218 |
As you would expect, my body temperature was a bit higher at night after a day of romping around (red line) than in the morning (blue line).
During this period, I ingested various amounts of a supplement called Thytrophin, earlier mentioned. I believe it helped with my tendon soreness and cold feet but did little, if anything, to improve my body temperature.
I’ll return to Thytrophin in the “My Protocol” section below.
So far we’ve examined why I think I have hypothyroidism. Next up is to get in an idea about what may cause a poor functioning thyroid and its effects.
Which Direction Is The Causality?
My hypothesis is that hypothyroidism is causing the various symptoms cited above, and those unfortunate blood markers, but what if it’s the reverse — that other stuff is causing my hypothyroidism?
That might be Chris Kresser’s take on the matter. He’s an acupuncturists, a practitioner of integrative medicine, and the writer of an ebook called Thyroid Disorders, which you can get free on his website here.
In Thyroid Disorders, Mr. Kresser digs into various causes or amplifiers (my word) of hypothyroidism. Turns out, in his examination of the issue, he reverses the causality posited by my hypothesis.
I’ve assumed that the unhealthy blood markers reported in Part 1 have weakened my thyroid, causing it to produce insufficient thyroid hormone; whereas, Chris Kresser takes the opposite perspective, mostly — that hypothyroidism causes (is not caused by) these conditions.
Let’s examine his views as presented in Thyroid Disorders, and summarized below by me for your delight. Chris Kresser’s info will be indented, and I hereby publicly apologize to him for any misrepresentation that may occur due to my paraphrasing, summarizing and interpenetrating.
Beneath each section presenting Mr. Kresser’s information, I’ll add “My Verdict” about whether I deem it applicable to my situation.
OK, here we go with nine potential causal agents for hypothyroidism per Chris Kresser’s ebook, Thyroid Disorders:
#1 Hypothyroidism Caused By Pituitary Dysfunction
This causality pattern suggests that an infection, blood sugar imbalances, insulin resistance, chronic stress, pregnancy or hypoglycemia is caused by elevated cortisol. These stressors fatigue the pituitary gland (located at the base of the brain) so that it can no longer signal the thyroid to release a proper amount of thyroid hormone.
In this case, there may be nothing wrong with the thyroid gland itself – the issue is that the pituitary isn’t sending it the right messages. With this pattern, you’ll have hypothyroid symptoms and a TSH below the functional range (1.8 – 3.0) but within the standard range (0.5 – 5.0). The T4 will be low in the functional range (and possibly the lab range too).
My Verdict: I have no idea what’s up with my pituitary gland, but my temptation is to eliminate persistently high cortisol as a contributing factor because I passed a self-administered four-part adrenal fatigue test, which I wrote about here (with video).
#2 Under-conversion of T4 to T3
T4, the inactive form of thyroid hormone, must be converted to T3 before the body can use it. T4 is 90% of thyroid hormone produced.
The under-conversion of T4 to T3 is caused by inflammation and elevated cortisol levels.
T4 to T3 conversion happens in cell membranes. Inflammatory cytokines damage cell membranes – where the T4 to T3 conversion occurs — and thus impairs the body’s ability to make the conversion happen. High cortisol also suppresses the conversion of T4 to T3.
With this pattern hypothyroid symptoms exist, but TSH and T4 will be normal. T3, however, will be low.
My Verdict: As reported in Part 1, my blood test indicates systemic inflammation (high C-reactive protein), but since I did not test T4, T3 or cortisol, I don’t know if these are contributing factors. Also, as mentioned, I passed this four-part adrenal test.
#3 Hypothyroidism Caused by Elevated TBG
Thyroid binding globulin (TBG) is the protein that transports thyroid hormone through the blood.
When TBG levels are high, levels of free thyroid hormone will be low, and visa versa as we’ll see next.
When thyroid hormone is bound to TBG, it is inactive and unavailable to the tissues. When TBG levels are high, levels of unbound (free) thyroid hormone will be low, leading to hypothyroid symptoms.
With this pattern, TSH and T4 will be normal. If tested, T3 will be low, and T3 uptake and TBG will be high.
Elevated TBG is caused by high estrogen levels, which are often associated with birth control pills or estrogen replacement. To treat this pattern, excess estrogen must be cleared from the body.
My Verdict: Am doubtful that this is an issue for me given that my estrogen number (19.3 pg/mL) is good for a male.
#4 Hypothyroidism Caused by Decreased TBG
This is the mirror image of the pattern above: Here TBG levels are low and levels of free thyroid hormone will be high.
Counterintuitively, the high free thyroid hormone in this instance does not reverse hypothyroidism nor cause hyperthyroidism (too much thyroid hormone) because cells become resistant to this high level of free thyroid hormone in the bloodstream. The result is hypo, not hyperthyroidism, symptoms.
With this pattern, TSH and T4 will be normal. If tested, T3 will be high, and T3 uptake and TBG will be low.
Another point here: Decreased TBG may be caused by high testosterone levels.
In women, it is commonly associated with Polycystic ovary syndrome (“PCOS”) and insulin resistance. Reversing insulin resistance and restoring blood sugar balance is the key to treating this pattern.
My Verdict: My testosterone and related numbers in my blood test are on the low side of the Reference Interval, so I rule out high testosterone decreasing TBG.
#5 Thyroid Resistance
In this case both the thyroid and pituitary glands are functioning normally, but the hormones aren’t getting into the cells where they’re needed, thus causing hypothyroid symptoms.
Note that all lab test markers will be normal in this pattern, because right now there’s no way to test the function of cellular receptors directly.
Thyroid resistance is usually caused by chronic stress and high cortisol levels. It can also be caused by high homocysteine and genetic factors.
My Verdict: Chronic stress and elevated cortisol levels will over time compromise the adrenal glands. I recently had myself videotaped doing four at-home tests for adrenal fatigue, which I passed, so I don’t think this is an issue for me.
#6 The Gluten/Thyroid Link
Mr. Kresser references five studies that link gluten sensitivity to autoimmune thyroid disease. I haven’t mentioned the “autoimmune” aspect of hypothyroidism, referred to as “Hashimoto’s disease”, but suffice to say that this is a condition whereby the immune systems attacks the thyroid. Not nice and very difficult to treat.
My Verdict: I seldom eat grains, but I do recognize that there’s nearly zero tolerance for gluten if you have a gluten allergy. If I do, surprised.
#7 Insufficient or Too Much Iodine
The prevailing wisdom is that most of us do not ingest enough iodine, a substance necessary for healthy thyroid function. Often then, the prescription for those with low-functioning thyroid is to take iodine.
Chris Kresser points out, however, that if your hypothyroidism is due to an autoimmune issue, supplementing with iodine increases the problem if you also have a selenium deficiency.
My verdict: I doubt I have an iodine deficiency as I supplement with spirulina powder and regularly eat seaweed. If I do have hypothyroidism and it’s from an autoimmune reaction, I should stop ingesting these iodine-rich foods… if, that is, I’m selenium-deficient.
#8 Selenium’s Affect on the Thyroid
Selenium is thought to improve thyroid function in those with autoimmune thyroid issues, perhaps by reducing the inflammation that damages thyroid tissue. Selenium is also essential for the conversion of T4 to T3, but should you start supplementing with selenium if you have hypothyroidism, Hashimoto’s thyroiditis, or low T3 levels?
It depends.
Preliminary studies show the positive effects of selenium supplementation on inflammatory activity in autoimmune thyroid conditions, but the long-term effects of supplementation on thyroid health are unknown.
My verdict: I eat four Brazil nuts each day. Assuming I’m ingesting the selenium in them, I should not be deficient; moreover, if this assumption is true, then (as above stated) the iodine I ingest should not be adding to my potential thyroid problem.
As a preamble to the forthcoming #9, know this…
Chris Kresser splits the blood sugar and thyroid dance into two sections in his Thyroid Disorders, but I’m combining them because I want to emphasis this predicament of multi-directional causality.
Again, what I mean by this comes down to the age old “chicken or egg” question, as in “which came first”.
Specific to my case, presuming I do have hypothyroidism (my hypothesis), did it cause my high blood sugar (given that my diet is stellar), or the reverse — did my high blood sugar cause (augment) my hypothyroidism?
This conundrum gets particularly thorny given that both my father and uncle got adult-onset (type 2) diabetes in their 60s, and my mother and sister have hypothyroidism.
The thorns prick the question: genetics or behavior?
In my case, I want to rule out behavior (diet/exercise/mindfulness) given that mine is inconsistent with habits associated with high blood sugar.
If genetics is the culprit, it would mean that it wasn’t only the lousy diet and lack of exercise that instigated my father and uncle’s diabetes, but that they had a genetic predisposition to it.
In the case of my mother and sister’s hypothyroidism… well, it might just come down to pounds, lots of them, and the metabolic syndrome thereby ignited. Nuff said.
#9 How High Blood Sugar Affects the Thyroid and Visa Versa
High blood sugar affect the thyroid like this:
The pancreas makes insulin whose function it is to remove excess glucose from the blood into cells where it (the glucose) is then used for energy. A high glycemic carb-rich diet produces too much glucose, which makes the pancreas produce too much insulin.
Kresser says that over time this excess insulin destroys the thyroid gland of those with autoimmune disease. I don’t know what this means for those whose thyroid issues do not stem from an autoimmune problem.
Conversely, low thyroid function affects blood sugar like this:
- It slows the rate of glucose uptake by cells
- It decreases the rate of glucose absorption in the gut
- It slows the response of insulin to elevated blood sugar
- It slow the clearance of insulin from the blood
These effects of low thyroid function “present clinically as hypoglyemia”, says Kresser, and:
When you’re hypothyroid, your cells aren’t very sensitive to glucose. So although you may have normal levels of glucose in your blood, you’ll have the symptoms of hypoglycemia (fatigue, headache, hunger, irritability, etc.). And since your cells aren’t getting the glucose they need, your adrenals will release cortisol to increase the amount of glucose available to them. This causes a chronic stress response […] that suppresses thyroid function.
(Source)
My verdict: This one’s got me by the throat. For reasons beyond my reckoning, my fasting blood sugar is high.
My Protocol to Combat Hypothyroidism (thus far)
What’s been presented up to this point is this:
- A brief look at some conclusions carried forward from Part 1, a blog post wherein I tried to chase down why various blood results indicate that I may be in declining health, a status inconsistent with my behavior and appearance.
- A presentation in support of why I think I have hypothyroidism, or at least some of the symptoms.
- A review of health conditions and mechanisms — as guided by Chris Kresser’s ebook, Thyroid Disorders — pertinent to hypothyroidism.
Now, let’s turn to what I’ve done to improve that embattled butterfly-looking gland that sits in my throat.
Thytrophin PMG
Until recently, Thytrophin could be purchased on Amazon.com. It had gotten high marks from various thyroid-focused web sites and doctors. The comments on Amazon where overwhelmingly favorable.
I bought a bottle of 360 tablets and started taking two each day. Over the course of some months, my dosage increased to five.
I bought another bottle, but not via Amazon. It no longer shows up there. I bought the second bottle online at Utopia Silver Supplements.
There’s still some tablets in the bottle, but I’m taking a break from Thytrophin. As I said earlier, I think it helped with my cold feet and tendon soreness, but did nothing for my body temperature.
Nutri-Meds ThyroidHealth
The bottle came today in the post. I got the porcine version, as those hogs are biologically closer to us than cows (bovine version).
This product is dessicated porcine (or bovine) thyroid from grass fed animals wandering the hills and dales of New Zealand.
Typically, you need a prescription for dessicated glandulars, but perhaps because this company makes no claims about the product, other than that it’s a “supplement”, they’re able to sell it direct to consumers.
I took one capsule, 130 mgs, and will continue with one for a few days, then increase the amount slowly till my body temperature begins to average between 98.2 and 97.2 Fahrenheit.
Basically, I’ll be following the regimen suggested by Nutri-Meds. Which amounts to slowly increasing the dosage, and recording how you’re feeling each day.
The Typical Stuff
In addition to taking ThyroidHealth, I’ll continue exercising and eating righteous foods and get my eight hours of sleep, etc. At some point, another blood test, or something similar, will need to be done.
Your Takeaway
If you’re thinking, “This guy Joe is nuts for trying to figure out something so complicated on his own”, I say:
I agree!
I should find an excellent endocrinologist with a bent toward naturopathy and let him/her figure it out. And maybe I will if the Nutri-Meds’ ThyroidHealth dessicated porcine “supplement” doesn’t work.
In the meantime, I’ll continue experimenting and report to you once there’s something worth jawboning about.
Yes, that means there will be a “Part 3”. You’ll have plenty of time to rest up for it.
And, since this is “Your Takeaway”, may I suggest that you:
- Don’t rely on my summary of Kresser’s ebook. For one reason, there’s a lot more in it than I covered. If the thyroid’s your issue, get his ebook.
- Ensure that your adrenals are OK before addressing your thyroid, as is discussed here.
- Take it really slow if you wind up taking dessicated anything and are not under the care of a doctor. Baby steps. Hormones are powerful things and they can mess you up.
That’s it.
If you have a question or comment, post it in Comments below.
Last Updated on December 25, 2019 by Joe Garma