8 Risk Factors for Chronic Inflammation and What To Do About It
Unless you’re a healthy youngster you have inflammation of the chronic variety. It comes with age, poor diet and weight gain — and results in various degenerative diseases. Here are eight risk factors for chronic inflammation and what you can do about it.
NAME SEVEN of the ten top causes of death in America influenced by chronic inflammation?
Can’t do it?
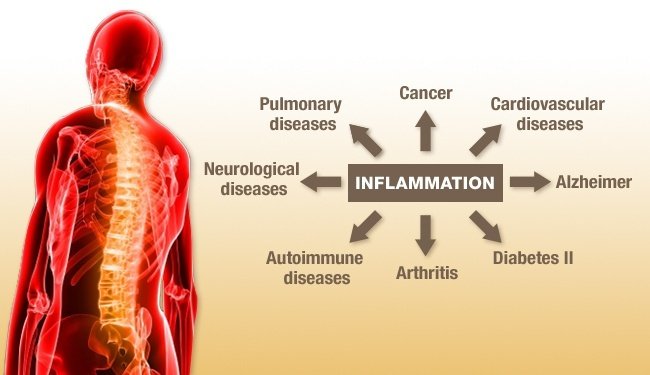
Well, I couldn’t either till I read the Life Extension Foundation inflammation protocol that said in the U.S., chronic, low-level inflammation contributes to the pathogenesis of these seven diseases:
- Heart disease
- Cancer
- Chronic lower respiratory disease,
- Stroke,
- Alzheimer’s,
- Diabetes, and
- Nephritis (kidney inflammation).
If that wasn’t enough, there’s one more nefarious thing that inflammation can do… prematurely age you! (As if that’s not happening quickly enough.)
Chronic inflammation can be triggered by cellular stress and dysfunction caused by excessive calorie consumption – particularly low glycemic/blood sugar spiking carbohydrates — elevated blood sugar levels (again, often do to excessive carb consumption), and oxidative stress.
Stress-induced inflammation can persist undetected for decades, causing cell death throughout the body. Due to the fact that it contributes so greatly to deterioration associated with the aging process, this silent state of chronic inflammation has been coined “inflammaging”.
That’s the danger of chronic, low-level inflammation — it’s silent but deadly.
And it’s happening to me.
A year ago, I had some blood work done and discovered that a marker for systemic inflammation — “C-Reactive Protein” — was high. Mine was 3.74 mg/L, above the “reference interval” of 0.0 – 3.0 mg/L.
This indicator of high systemic inflammation would be understandable if my habits approximated those that typically trigger this condition, but they aren’t. I’m currently investigating the root cause, which is outside the focus of this article, but suffice to say that one’s hormones need to be optimized, or a cascade of unhappy health events otherwise occur.
{Read The Poor Performing Hormone That May Cause Your Chronic Health Problems.}
The truth is, chronic inflammation is common and must be conquered in order for people to have a long and healthy life unperturbed by the many chronic diseases that are influenced by inflammation.
What I will cover in this article is this:
- Five biochemical inducers of inflammation-caused cellular stress,
- Eight risk factors for chronic inflammation, and
- What to do to become and anti-inflammatory paragon of virtuous health.
(Hint: it includes diet, supplements and blood.)
{This article is my second deep-dive about inflammation, the first called Six Simple Solutions To Rid Yourself of Inflammation, and it gets into some of my own issues with this pervasive health issue.}
To kick things off, let’s examine how inflammation happens in the body, and what are its markers and mediators.
The Acute Inflammatory Response
An inflammatory response is triggered when you get a tissue injury or an infection by viruses, bacteria, parasites or or the fungus among us. This is natural, normal, necessary and is termed “acute” because a certain sequence of biological responses needs to happen quickly to help heal the injury/infection.
A well-controlled acute inflammatory response has several protective roles, as it can:
- Prevent the spread of infectious agents and damage to nearby tissues;
- Help remove damaged tissue and pathogens; and
- Assist the body’s repair processes.
If all goes well, healing happens and the inflammation subsides.
But if the cause of the inflammation was cellular stress and malfunction, it may stick around, and rather than be beneficial, this chronic inflammation will contribute to disease and age-related deterioration.
Cellular Stress & Chronic, Low-Level Inflammation
There are basically five biochemical inducers of inflammation-caused cellular stress: mitochondria dysfunction, advanced glycation end products, uric acid, oxidized lipoproteins and homocysteine.
Let’s briefly look at them, and then examine the risk factors for chronic inflammation.
– Mitochondria dysfunction
Mighty mitochondria are the cellular organelles that make adenosine triphophate (“ATM”), which is the biochemical energy that makes life possible for multicellular life forms, like yourself, for instance.
Unfortunately, mitochondria are sensitive little organelles. They become dysfunctional when either some exogenous (environmental toxins) or endogenous (reactive oxygen species) stressors happen, or as a consequence of the aging process.
In fact, one substantial theory of aging concerns mitochondrial dysfunction due to free radical accumulation over time.
One byproduct of mitochondrial energy generation (ATP) is the creation of free radical molecules. Free radicals can damage cells and cause proinflammatory genetic signals that eventually results in cell apoptosis (death), or uncontrolled cell propagation; ie cancer.
– Advanced Glycation End Products
Sugars circulating in the blood stream, primarily glucose and fructose, contribute to inflammation as well.
When these “blood sugars” come in contact with proteins and lipids, a damaging reaction occurs forming compounds called advanced glycation end products (“AGEs”) which bind to certain cell-surface receptors that eventually activate numerous inflammatory genes.
The prevalence of AGEs is exacerbated by elevated blood sugar levels and in food cooked at high temperatures, especially seared red meat.
– Uric acid
These are crystals, which can be deposited in joints during gouty arthritis. Elevated levels are a risk factor for kidney disease, hypertension, and metabolic syndrome.
– Oxidized Lipoproteins
You’ve heard about lipoproteins in the context of cholesterol.
Your total cholesterol number is comprised of adding the “good” lipoprotein that you wan more of, HDL (“high-density lipoprotein”) to the “bad” lipoprotein that you want less of, LDL (“low-density lipoprotein”).
When lipoproteins are oxidized they become significant contributors to atherosclerotic plaques, a risk factor for cardiovascular disease.
– Homocysteine
This is a non-protein-forming amino acid that is a marker and risk factor for chronic inflammation and cardiovascular disease.
{To learn more about what causes inflammation and its markers and mediators, go here.}
Now that we have an appreciation for what induces persistent inflammation, let’s examine eight risk factors.
The 8 Risk Factors for Chronic Inflammation
There are several risk factors which increase the likelihood of establishing and maintaining a low-level inflammatory response, eight of which we’ll touch on here.
#1. Age
There’s a positive correlation between age and consistently elevated levels of several inflammatory molecules.
The younger you are the more probable that the inflammation experienced is acute, and occurs in reaction to a tissue injury or infection. As we get older, however, the inflammation experienced tends to be chronic, even in healthy individuals.
As mentioned above, the thinking here is that age-associated chronic inflammation is due to mitochondrial and oxidative damage, but other risk factors associated with age may also come into play, such as increases in body fat and reductions in sex hormones.
#2. Obesity
Have you heard the term, “the biology of blubber”?
It refers to the fact that fat is not inert, but rather has a biochemistry of its very own.
Fat tissue is an endocrine organ, storing and secreting multiple hormones and cytokines (small cell signaling proteins) into circulation and affecting metabolism.
Fat cells produce and secrete various inflammatory molecules, and visceral (abdominal) fat does this three times more than other fat cells. The amount of pro-inflammatory cytokines secreted is proportional to one’s Body Mass Index (“BMI”), an imperfect but fairly accurate measure of relative fatness. (Unless you’re very tall, small or muscular — check out BIG Tangent #1: BMI Can Be Misleading.)
#3. Diet
The science may be shifting on this but historically, studies indicate that a diet high in saturated fat is associated with higher pro-inflammatory markers, particularly in diabetic or overweight individuals.
What is still universally accepted among most who study such things is that diets high in synthetic trans-fats (such as those produced by hydrogenation) have been associated with increases in inflammatory markers.
That means a diet burdened by fast food and processed food will produce more chronic inflammation than a diet dominated by whole foods — the stuff that looks about the same in your fridge and cupboards as it does on the farm.
#4. Low Sex Hormones
Those good ole sex hormones do a lot of wonderful things, and among them is to modulate the immune/inflammatory response.
Neutrophils and macrophages are cells that mediate inflammation, and they have receptors for estrogens and androgens that enable them to selectively respond to sex hormone levels.
Various experiments and observational studies indicate that:
- Testosterone and estrogen can repress the production and secretion of several pro-inflammatory markers.
- Lower testosterone levels in elderly men increase inflammatory markers
- There can be an increase in inflammatory markers following surgical or natural menopause.
- The preservation of sex hormone levels is associated with reductions in the risk of several inflammatory diseases, including atherosclerosis, asthma in women, and rheumatoid arthritis in men.
- Reductions in the risks of coronary heart disease and inflammatory bowel disease in some individuals, as well as levels of some circulating inflammatory cytokines has been observed in some studies of women on hormone replacement therapy.
#5. Smoking
I live in a place just north of the Golden Gate Bridge where a person could pitter-patter around for a week and not see anyone lighting up. But I hear that elsewhere some people still inhale smoke into their lungs on a regular basis.
Well, if you know of anyone who does this sorta thing, let him/her/them know that cigarette smoke contains several inducers of inflammation, and reduces the production of anti-inflammatory molecules.
And one more goodie — Smoking also increases the risk of periodontal disease, an independent risk factor for increasing systemic inflammation.
That said, if you’re a committed smoker you have more to worry about than how chronic inflammation may manifest some degenerative disease.
#6. Periodontal Disease
Yes, this was mentioned above; suffice to say that periodontal (gum) disease can produce a systemic inflammatory response that may affect several other systems, such as the heart and kidneys, and thereby could be a risk factor for cardiovascular diseases.
#7. Sleep Disorders
People with irregular or disrupted sleep patterns may be more susceptible to chronic inflammation than those consistent, sound sleepers.
The production of inflammatory cytokines may follow a circadian rhythm and disruption of normal sleep can lead to daytime elevations of these pro-inflammatory molecules. This is true independent of BMI or age.
#8. Stress
Stress is a biggie.
It can shorten telomeres, and both physical and emotional stress can lead to inflammatory cytokine release.
As already pointed out, stress is also associated with decreased sleep and increased body mass (stimulated by release of the stress hormone cortisol), which are each independent causes of inflammation.
{To learn more about risk factors for chronic inflammation and the research behind the assertions made above, go here.}
Conventional Doctors Overlook Chronic Inflammation
Before you began reading this article, you undoubtedly were aware of – and perhaps even experienced — some of the various diseases mentioned, but did you have an appreciation for how significant is inflammation’s role in instigating those disease states?
Perhaps not, and maybe the reason is that conventional medical types are not dialed into chronic inflammation, and thus your doctor hasn’t spoken to you about it.
They typically get focused on the disease, not what lead to it.
Certainly, I didn’t have a clue that I might have chronic inflammation. I do not engage in the behaviors that can lead to inflammation, nor am I experiencing any of the potential diseases it can influence (yet).
Thankfully, a blood test I did administrated by Life Extension Foundation to measure my testosterone and other steroid hormones was comprehensive enough to include C-Reactive protein, a blood marker for chronic inflammation.
If you may be susceptible to chronic inflammation, you may want to test for it.
Testing Blood for Inflammatory Factors
The following two blood tests are inexpensive and are good markers of systemic inflammation. They can be used to detect the presence of chronic inflammation and monitor the success or failure of various anti-inflammatory regimens:
| Pro-Inflammatory Marker | Optimal Ranges |
| High-sensitivity C-reactive protein (CRP); | Under 0.55 mg/L in men |
| Under 1.0 mg/L in women | |
| Fibrinogen | 200 – 300 mg/dL |
The following blood tests are expensive and help identify specific factors that are causing systemic inflammation:
| Cytokine Testing | Normal Ranges (LabCorp) |
| Tumor necrosis factor alpha (TNF-α) | <8.1 pg/mL |
| Interleukin-1 beta (IL-1β) | <15.0 pg/mL |
| Interleukin-6 (IL-6) | 2-29 pg/mL |
| Interleukin-8 (IL-8) | <32.0 pg/mL |
To learn more about Life Extension Foundation’s test for inflammation, click on the image below:
Nutritional Approaches to Reduce Chronic Inflammation
You now know the risk factors for inflammation and can therefore get a sense if you’re vulnerable.
If you are, you can find out about getting a blood test by clicking the image above.
-> Now, let’s check on various nutrients, dietary factors and the like that can help reduce chronic inflammation.
Macronutrients and Energy Balance
Macronutrients are proteins, fats and carbohydrates.
To minimize inflammation (and get a secondary benefit of overall good health to boot) do this:
- Consume high quality fats
- Eat primarily low glycemic carbs
- Get most of your protein from fish and vegetable sources
High quality fats include walnuts, pecans, Brazil nuts, almonds, omega-3 fatty acids and monounsaturated fatty acids (avocado, flax seeds, chia seeds, hemp seeds, fish oil and high quality, cold pressed, extra virgin olive oil).
Low glycemic carbs are those that digest slowly and thus do not spike your blood sugar. Stay away from white pasta, white rice, white bread, fruit juice and processed foods and you’ll be fine. For more about glycemic index and load read this.
Some good protein sources include salmon, sardines, trout, herring and lentils.
Dr. Andrew Weil has an anti-inflammatory diet you can read about here, which has its very own pyramid:
Fiber
Ingesting both soluble and insoluble fiber can reduce chronic inflammation, not to mention dramatically improve gut health and curb your appetite by helping to make you feel full.
Soluble fiber attracts water and form a gel, which slows down digestion. Sources include oatmeal, oat cereal, lentils, apples, oranges, pears, oat bran, strawberries, nuts, flaxseeds, beans, dried peas, blueberries, psyllium husk powder, cucumbers, celery, and carrots.
Insoluble fiber does not dissolve in water, so it passes through the gastrointestinal tract relatively intact, and speeds up the passage of food and waste through your gut. Sources include whole wheat, whole grains, wheat bran, corn bran, seeds, nuts, barley, couscous, brown rice, bulgur, zucchini, celery, broccoli, cabbage, onions, tomatoes, carrots, cucumbers, green beans, dark leafy vegetables, raisins, grapes, fruit, and root vegetable skins.
Vitamins/mineral/plant supplements with anti-inflammatory properties include:
- Magnesium
- Vitamin D
- Vitamin E
- Zinc
- Selenium
- Resveratrol
- Curcumin
- Tea polyphenols
- Carotenoids
- DHEA
- Fish Oil
- N-acetyl cysteine (NAC)
- Boswellia
- Sesame Lignans
- Bromelain
- Coenzyme Q10 (CoQ10) and
- Pyrrloquinoline Quinone (PQQ)
- Carnosine
- Benfotiamine
{To learn more about inflammation-reducing nutrients and drug strategies, particularly the research behind the assertions made above, go here and here.}
Yes, that’s quite a list, and it’s a bit intimidating. Which brings me to the next and last section of this article…
Take These 5 Steps to Reduce Chronic Inflammation
I’ve given you a lot to chew on here, and it can seem overwhelming, so let’s this down into some actionable steps.
No, this is not gonna kill you. Just the opposite!
1. Assess if chronic inflammation is an issue for you.
If you’re younger than 40, healthy and eat plenty of fiber, fruits and vegetables and have no aches and pains, just keep at it.
If you’re stiff and sore, have health issues, are overweight and/or are over 40, move on to #2.
2. Review those 8 “risk factors” listed above.
If one or more apply to you, go to #3.
3. Get a blood test for inflammation.
If you test high for chronic inflammation you should consult with your doctor about it. You can also take some further steps…
4. Modify your diet per Dr. Weil’s Anti-inflammatory Diet described above.
You can take this step-by-step as well. One’s diet is a big deal. You don’t change it whole hog overnight, but by small, progressive steps.
5. Start with a high quality multivitamin/mineral and a good curcumin supplement as well.
I use Extinguish and Optimized Curcumin, both offered by ProHealth:
Over time, add some of the other supplements listed above.
Life Extension Foundation is another source for a large selection of anti-inflammation supplements. Click on Life Extension Products and use the word “inflammation” in the search box. You’ll get something that looks like this:
Remember that reducing your chronic inflammation is a huge step to avoiding the many behavior-related disease states that dramatically reduce our quality of life, particularly if they kill us.
So, get going.
Over and out.
P.S. If you’d like to stay up to date about new articles and learn how I will eventually beat my own chronic inflammation into submission, please join my weekly Newsletter.
Last Updated on February 28, 2022 by Joe Garma